This is something that I continue to hear from time to time even in 2020 and I imagine I will continue to hear rumblings about this in 2022. Certainly, there are physical limitations when a baby is born at less than 500g. Have you tried fitting a mask to deliver NIPPV or CPAP to a baby this small? I have and it didn’t work. The mask was simply too big to provide a seal and while I am all for INSURE and emerging minimally invasive surfactant techniques they still require transitioning to a form of non invasive positive pressure ventilation to allow extubation success. Certainly though above the 500g barrier it may be that the greatest impediment to extubation is our own bias.
If this sounds a little familiar it is because I have written about this topic before Extubation failure is not a failure itself. The reason for bringing the topic up again though is that aside from needing to address our own fears there is a new systematic review that acts somewhat of a how to guide to optimizing your chance at a successful extubation. The review encompasses findings from 50 studies with successful extubation as defined as no need for reintubation within 7 days. Before getting into the details of the optimal approach it is worth reminding people that failure of extubation in even our smallest babies is not a failure itself. Such babies who “fail” up to 5 times do not suffer any long term consequences and may wind up with less risk of BPD than those who are kept intubated due to fear of failure.
So After Reviewing The Evidence What Are the Recipes To Success?
-
-
Continuous positive airway pressure
Reduced extubation failure in comparison with head-box oxygen (risk ratio [RR], 0.59;95%CI, 0.48-0.72; number needed to treat [NNT], 6; 95%CI, 3-9). If you aren’t extubating to nCPAP then chances are I would bet your success rates are quite low. Head boxes certainly can tell you how much O2 a patient requires but do nothing to help inflate alveolar spaces.
-
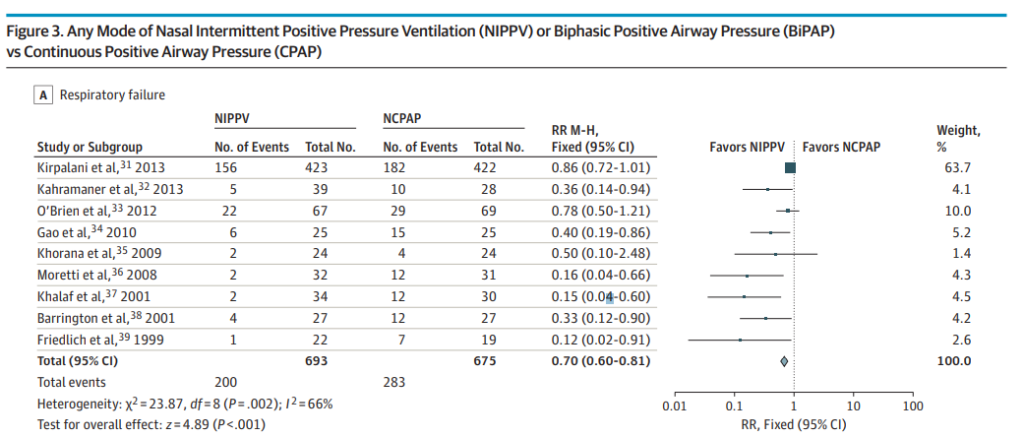
Nasal intermittent positive pressure ventilation (NIPPV) vs. CPAP
Higher prevention of extubation failure (RR, 0.70; 95%CI, 0.60-0.81; NNT, 8; 95%CI, 5-13). This one is of particular interest to me. The evidence has suggested this for some time and with a number needed to treat of 8 it would seem illogical to use anything else at the outset, especially in the smallest of infants. The issue here though is that at least here in Canada the options for delivering such NIPPV are currently quite limited. At the moment we are limited to use of ventilator NIPPV and the stability of the CPAP offered from such devices and the imposed work of breathing are most likely inferior to that found in variable flow devices which at this point have been pulled from the market. See Comparison of nasal continuous positive airway pressure delivered by seven ventilators using simulated neonatal breathing. What I hope 2017 brings is a comparison of the effectiveness of extubation success using new variable flow devices capable of generating previously unreachable CPAP pressures above 9 or 10 cm H2O. Will these attain similar effectiveness to the NIPPV devices? Forrest plot below
-
Methylxanthines reduced extubation failure (RR, 0.48; 95%CI, 0.32-0.71; NNT, 4; 95%CI, 2-7) compared with placebo or no treatment. Ok, pretty much anyone working in Neonatology would assume this but what really is at the crux of the discussion in 2016 and beyond is “what dose?” It has been pretty clear during my career thus far that there are some preterm infants that just don’t respond to conventional doses of caffeine base from 2.5 – 5 mg/kg/d. In our own units we have increased doses to 6, 7 or 8 mg/kg/d to achieve some degree of respiratory stimulation and usually been limited by tachycardia in determining how high we can go. Given the sparse literature regarding safety on this topic we are relegated to ask ourselves what is worse, leaving a baby on a ventilator or using higher doses of caffeine? I have given some thoughts on this before as well Are we overdosing preemies on caffeine?
-
Doxapram did not aid successful extubation (RR, 0.80; 95% CI, 0.22-2.97). For selfish reasons I have to admit I was happy to see this. We can’t access this medication very easily here in Canada so hearing that it doesn’t seem to work to enhance the likelihood of a successful extubation is somewhat of a relief.
-
A Cautionary Note
While I applaud the authors of the systematic review for performing such a thorough job I do feel the need to raise one concern with the analysis. It is not a major concern but one that I just feel the need to mention. Success if the studies was defined as not requiring reintubation within 7 days of extubation. My concern is that having such a lengthy time frame leaves the possibility that the decision to reintubate had nothing to do with the patient in fact not being ready. Seven days is a long time and much can happen in the life of a preterm infant in an NICU that triggers a reintubation. What if a patient needed to be transferred to a different NICU and for safe air transport it was deemed safest to replace the ETT? How many patients could have developed NEC or sepsis in the seven days? What if a PDA was being semi-electively ligated after a failed NSAID course?
In the end the impact of such conditions could be minimal but I am less convinced that a patient failed extubation when up to 7 days have passed. I would be very interested to see a similar study looking at a period of 24 or 48 hours after extubation and seeing how many stay that way. Would the predictors of success stay the same? Probably but I suspect the number safely extubated would rise as well.


True….
Most of us suffer from the bias “too small to extubate”.
Many of us do unnecessarily worry about the extubation failure.
I admire the way author has put his view.
Can we be a bit holistic, when we decide to intubate.
Can we afford to think, “too small to intubate”.
It was a pleasure to read you. My experience with larger babies (1000g and more) is that endotracheal tube is pathologic by itself. It is worth trying to extubate (on CPAP, NIPPV and as I just learned, high doses caffeine). I think that one point is important: we must be quick to recognize the failure of extubation and resume invasive PPV (with APRV?).
yes I think that it is imperative that when your decision turns out to be incorrect that you support the neonate with that which they need. Quite often due to volume loss that need is higher in terms of peep than was used before the extubation but this can be gradually weaned after FRC is restablished