
by All Things Neonatal | Jun 27, 2018 | NAS, Neonatal, neonatal abstinence, Neonatology
 This post is very timely as the CPS Fetus and Newborn committee has just released a new practice point:
This post is very timely as the CPS Fetus and Newborn committee has just released a new practice point:
Managing infants born to mothers who have used opioids during pregnancy
Have a look at discharge considerations as that section in the statement speaks to this topic as well!
As bed pressures mount seemingly everywhere and “patient flow” becomes the catch-word of the day, wouldn’t it be nice to manage NAS patients in their homes? In many centres, such patients if hospitalized can take up to 3 weeks on average to discharge home off medications. Although done sporadically in our own centre, the question remains is one approach better than the another? Nothing is ever simple though and no doubt there are many factors to consider depending on where you live and what resources are available to you. Do you have outpatient follow-up at your disposal with practitioners well versed in the symptoms of NAS and moreover know what to do about them? Is there comfort in the first place with sending babies home on an opioid or phenobarbital with potential side effects of sedation and poor feeding? Nonetheless, the temptation to shift therapy from an inpatient to outpatient approach is very tempting.
The Tennessee Experience
Maalouf Fl et al have published an interesting account of the experience with outpatient therapy in their paper Outpatient Pharmacotherapy for Neonatal Abstinence Syndrome. The authors were able to take advantage of the Tennessee Medicaid program using administrative
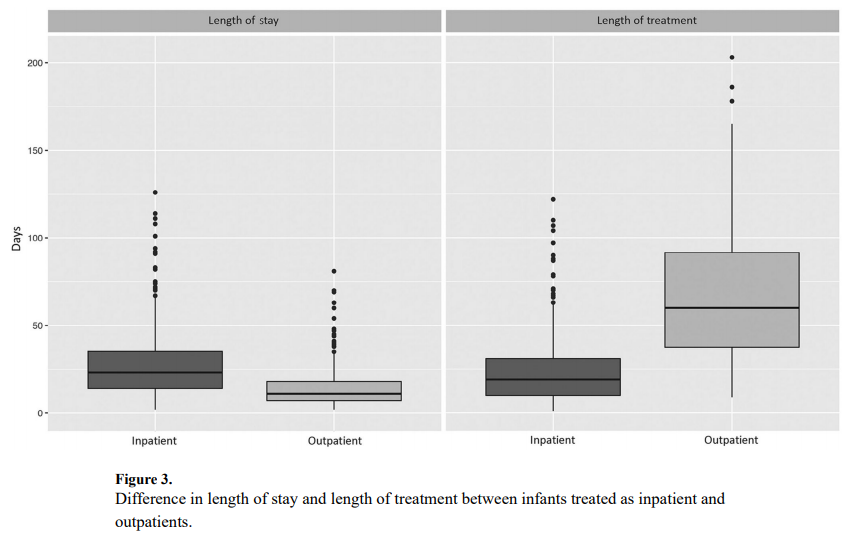
and vital records data from 2009 to 2011 to capture a cohort of 736 patients who were treated for NAS. Forty five percent or 242 patients were treated as outpatients vs 290 cared for in hospital for the duration of treatment. It is worth mentioning at this point that when the authors say they were cared for as outpatients it really is a hybrid model as the duration of hospitalization for the inpatients was a median of 23 days (IQR 14-35) versus 11 days (IQR 7-18) for inpatients (P < .001). This practice isn’t much different than my own in which I start therapy in hospital and then discharge home with a period of home therapy.
The strength of the study is the volume of patients and the ability to follow-up with these babies for the first 6 months of life to determine what happened to them after discharge. In terms of duration of treatment, the differences are significant but perhaps not surprising. The median length of treatment for outpatients was 60 days (IQR 38-92) compared with 19 days (IQR 10-31) for inpatients (P < .001). What was interesting as well is that 82% of babies were discharged home on phenobarbital and 9.1% on methadone and 7.4% with both. A very small minority was discharged home on something else such as morphine or clonidine. That there was a tripling of medication wean is not surprising as once the patients are out of the watchful eye of the medical team in hospital it is likely that practitioners would use a very slow wean out of hospital to minimize the risk of withdrawal.
An Unintended Consequence
This study found a statistically significant increase in risk for presenting to the emergency department for those patients treated as outpatients.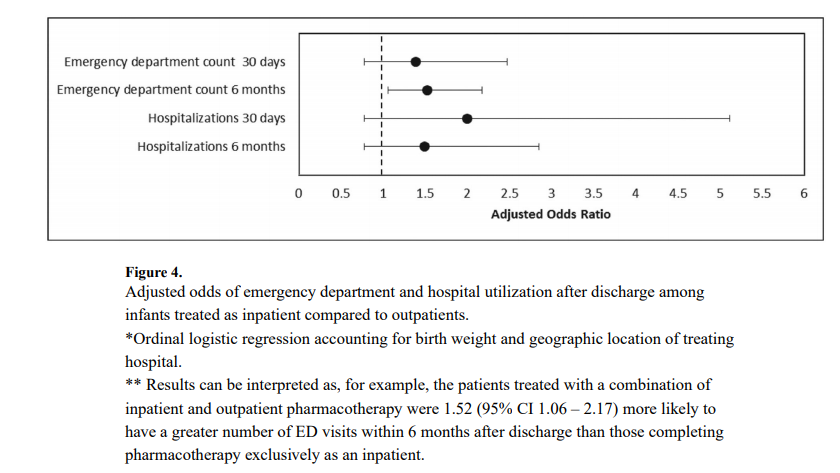

What this graph demonstrates is that there was no increase risk in the first month but there was for the first 6 months. Despite the increased risk of presentation to the ED the rate of hospitalization was not different. Drilling down the data further, the reason for coming to the ED was not for withdrawal which was 10% in the outpatient and 11% in the inpatient group. The other major reason was The most common diagnoses were upper respiratory infections; 80% outpatient vs 71% inpatient. So while there was a significant difference (which was not by much) my take on it is that it was most likely by chance as I can’t think of how infections in the first 6 months could be linked to choice of medication wean.
What about phenobarbital?
Phenobarbital has been used for many years in Neonatology for control of seizures, sedation (taking advantage of a side effect) and management of NAS. The problem with a median use of phenobarbital for 2 months is its potential to affect development.

An animal study by Diaz in 1999 in which rat pups were given two weeks of phenobarbital starting on day 5 of life and then euthanized demonstrated the following weight reductions when high dose phenobarbital was utilized. In human data, children with febrile seizures treated with phenobarbital in the paper Late cognitive effects of early treatment with phenobarbital. had decreased intelligence than those not exposed to phenobarbital.
The issue here for me is not necessarily whether babies can be treated successfully as outpatients for NAS. The concern is at what cost if the choice of drug is phenobarbital. The reason phenobarbital was chosen is likely due to compliance. We know that the more frequently a drug is dose the less likely compliance will be achieved. Phenobarbital being dosed either q12h or q24h is an ideal drug from a compliance point of view but the ramifications of this treatment deserve reconsideration.
I look forward to seeing further studies on this topic and hope that we see the results of an opioid outpatient treatment program. I know these exist and would welcome any information you as the readers of this blog can offer. Treating patients in the home makes great sense to me but we need to do it with the right drugs!

by All Things Neonatal | Jan 11, 2018 | NAS, Neonatal, neonatal abstinence, Neonatology, preemie
I wish it were otherwise, but in my practice, I have seen a growing number of pregnancies complicated by signs of substance withdrawal in newborn babies. Print, online, and broadcast news sources include regular reports on the “opioid crisis”. Data from the Canadian Institute for Health Information indicate that in 2016-17, about 1 in 200 newborns in Canada were affected by symptoms of drug withdrawal after birth. As this represents an average, there are no doubt some centres with much higher rates, while others may seem far lower depending on local usage patterns. Wherever you practice, if you care for newborns, you must learn how to treat this.
If you ask a physician in training how best to treat such conditions, their first response is often to use a medication such as morphine, thinking that it is best to treat an opioid withdrawal with the same class of drug. While this may be true, it is important to note that beginning with something much simpler, if not more natural, may reap tremendous benefits.
The Canadian Pediatric Society (CPS) released a new practice point this week, Managing infants born to mothers who have used opioids during pregnancy. While the document addresses the use of medical treatment, it highlights something far more important. Think of managing such pregnancies as a pyramid, with substance avoidance (the best strategy) on the bottom. The next level would be to manage newborns by keeping mothers and babies together. The top of the pyramid—that is, the fewest number of cases—would be treating these babies with medications.
For many families, avoidance is just not possible. Whether mothers use opioids due to addiction or chronic pain, it is simply unsafe to quit cold turkey. In October 2017, the Society of Obstetricians and Gynaecologists (SOGC) recommended against opioid detoxification in pregnancy because of the high risk of relapse. We should commend pregnant women who take responsibility for their health and seek care to stabilize on medications such as methadone or buprenorphine to manage their symptoms. After delivery, though, taking these babies and placing them on medications in a special care nursery should be a last resort.
Getting back to nature
Medications do work, but giving them means admitting babies to special care nurseries. This forced separation from families and, in particular, their mothers, actually leads to longer stays in hospital. Skin-to-skin care and breastfeeding contribute to better bonding between mother and child and have been associated with shortened hospital stays. In our centre, we have seen great success with many infants managed for up to seven days on the post-partum ward with their families. While this may seem like a long time, it is less than half of the average 15-day stay when babies are admitted to a special care unit.
Provided a mother is HIV-negative, the benefits of breastfeeding may go well beyond the bonding and closeness associated between mother and newborn. As most of these women continue to use a substance to ease their own withdrawal or pain, the small quantities of opioid that enter the breastmilk are in turn passed on to the newborn, which helps ease them through this transitional period in their life.
As the saying goes, sometimes less is more. In the case of caring for newborns exposed to opioids in pregnancy, getting back to nature and promoting skin-to-skin care and breastfeeding is just what this doctor ordered.

by All Things Neonatal | May 11, 2016 | drug withdrawal, NAS, Uncategorized
Original Post
I don’t know if you missed it but I did until tonight. We don’t have this in Canada but there have been some US states that have been doing so for the past while. You may find the following link very interesting that explains the positions of each state in regards to drug use in pregnancy. The intentions were good to protect the unborn child but the consequences to mother’s who tested positive were of great concern. While testing of mothers for drug use has been done off and on for years what made this different was that the confirmation of drug use was deemed to be a criminal offense with the results handed over to the police.
As this article from March 4th indicates the practice has been ongoing in Tennessee for at least a year and a pilot project was planned for Indiana this year. According to the article the situation in Tennessee came with some significant risk to the mother if found to have a positive screen.
“Lawmakers in Tennessee last year increased drug screenings of expectant mothers and passed a law allowing prosecutors to charge a woman with aggravated assault against her unborn baby if she was caught using illicit drugs. The penalty is up to 15 years in prison.”
The law may seem harsh and in my eyes is but it came in response to the tidal wave of drug addiction and neonatal withdrawal in the US as was identified in the article from the NEJM in 2015 entitled Increasing Incidence of the Neonatal Abstinence Syndrome in U.S. Neonatal ICUs. The impact on neonatal ICUs in the US can be seen in the following graphs which demonstrate not only the phenomenal rise in the incidence of the problem but in the second graph the gradually prolonging length of stay that these patients face. 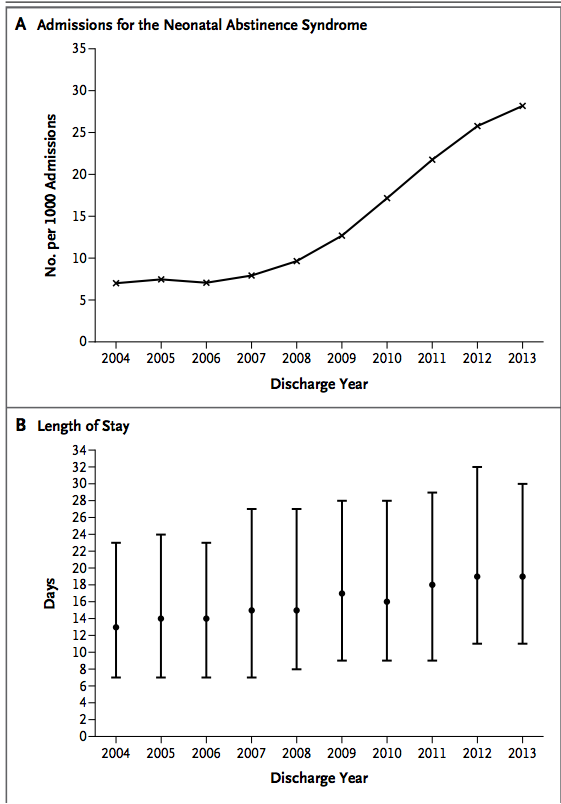 Aside from the societal issues these families face and the problems their infants experience, the swelling volume of patients NICUs have to contend with are quite simply overwhelming resources with time. Although I reside in Canada, it is the trend shown that likely motivated some states to adopt such a draconian approach to these mother-infant dyads.
Aside from the societal issues these families face and the problems their infants experience, the swelling volume of patients NICUs have to contend with are quite simply overwhelming resources with time. Although I reside in Canada, it is the trend shown that likely motivated some states to adopt such a draconian approach to these mother-infant dyads.
There are so many questions that would arise from such an approach.
- What if a mother refuses testing as is the option in Indiana. Would Child and Family services be called simply on the suspicion?
- What if a mother received prescription opioids for chronic back pain or used an old prescription in the days before she was tested after a fall to ease her pain?
- Then there is the Sharapova situation
 where a mother could conceivably take a medication that she is unaware is on a list of “banned substances”. What about Naturopathic or herbal supplements that might test positive?
where a mother could conceivably take a medication that she is unaware is on a list of “banned substances”. What about Naturopathic or herbal supplements that might test positive?
- Then what about false positive tests?
The ramifications of any of the above situations on the family unit could be devastating. Interestingly this year the courts in Indiana passed a law that prevents health care providers from releasing the results of such toxicology screens to police without a court order so indeed there would need to be suspicion. In the end though is it right?
Tennessee Sings a New Tune
As surprised as I was to hear about the situation in Tennessee just now I was equally surprised to come across a U.S. Supreme Court ruling handed down March 21st, 2001 that has ruled that subjecting mothers to such testing in hospitals is unconstitutional. This may disclose my ignorance of US law but I would have thought if the US Supreme Court says you cannot do something the states would follow along but at least in Tennessee that was not the case…until now.
March 23rd the law in Tennessee is changing as the state has chosen not to renew the legislation after a two year trial period saw about 100 women arrested. For more information on this decision see Assault Charges for Pregnant Drug Users Set to Stop in Tennessee.
Where do we possibly go from here?
I found this whole storyline shocking but I am taking some solace in knowing that this was a very limited experiment in one state. Neonatal abstinence is a problem and a big one at that. Criminalizing mothers though is not an effective solution and to me the solution to this problem will need to involve a preventative approach rather than one of punishment. A first step in the right direction will be to stem the tide of liberal use of prescription opioids in pregnancy as was suggested in the BMJ news release in January of this year. In the end if we as medical practitioners are freely prescribing such medications to the mothers we care for perhaps we should look in the mirror when pointing fingers to determine fault. So many of the mothers and the infants we care for may well be victims of a medical establishment that has not done enough to prevent the problem.
Update
While screening women presenting to the hospital in labour or their newborns for that matter may seem like a wise choice, the request to procure a sample remains just that. It is a request and in collecting consent is needed. This was the advice at least I was given by the Canadian Medical Protective Association. It does create an interesting situation though in the mother who refuses to have her or her baby submit a urine specimen. Should we assume that a woman who refuses testing is in fact using an illicit substance or is she merely choosing to not have a wasted test when she knows that she is not using anything? How do we as practitioners view this decision and do we jump to a verdict of guilt immediately? I suspect the answer is that most of us would assume so especially if we are using a targeted screening approach in which we are only approaching those mothers who we suspect are using.
The secondary question becomes the “so what”? What I mean by this is how will our management change if we know or don’t know? If we suspect use and the baby is demonstrating signs of withdrawal abstinence scoring will start. If the source of the symptoms are unknown would we not just treat with phenobarbital to cover the possibility that there is more than one drug at play here? I used to be on the side of the argument that felt we had to know and therefore pushed for such screening but in the end will it really change our management? Not really.
This past month the American College of Obstetricians and Gynecologists (ACOG) issued a committee opinion on opioid use in pregnancy. The important points to share with you are the following and I would agree with each.
- Screening for substance use should be part of comprehensive obstetric care and should be done at the first prenatal visit in partnership with the pregnant woman. Screening based only on factors, such as poor adherence to prenatal care or prior adverse pregnancy outcome, can lead to missed cases, and may add to stereotyping and stigma. Therefore, it is essential that screening be universal
- Urine drug testing has also been used to detect or confirm suspected substance use, but should be performed only with the patient’s consent and in compliance with state laws.
- Breastfeeding should be encouraged in women who are stable on their opioid agonists, who are not using illicit drugs, and who have no other contraindications, such as human immunodeficiency virus (HIV) infection. Women should be counseled about the need to suspend breastfeeding in the event of a relapse.
The issue of consent seems to be firmly in place based on this position and as I mention above I think that is a good thing. The question of breastfeeding comes up frequently and it is good to see ACOG take a clear view on this as I have often thought that the benefits of the same plus the administration of small quantities of the drug in the milk may have a double benefit in reducing symptoms.
.
by All Things Neonatal | Dec 11, 2015 | NAS
As anyone who has been reading this blog knows, I have an affinity for anything that is non-invasive and improves the care of newborns. Add to this my interest in Neonatal Abstinence (which has been the focus of other pieces such as Long term cognitive deficits in infants exposed to in-utero opioids and polysubstance use. In a rare finding, girls may have worse outcomes.) and a recent report of laser acupuncture for adjuvant treatment of neonatal abstinence syndrome would have to pique my interest. In 2014 a case report entitled Laser acupuncture as an adjuvant therapy for a neonate with neonatal abstinence syndrome (NAS) due to maternal substitution therapy: additional value of acupuncture. was published by Raith. I recall seeing this paper prior to starting this blog and Facebook page and made a mental note to check it out someday. That someday is upon me now that an RCT has been published on the subject which will be looked at below.
What is laser acupuncture?
Before we get into critiquing such a study it is worth explaining what laser acupuncture is. From the website acupuncture today I found the following background:
“In 1991, a study was done in Novosibirsk, Russia that applied directly to the study of acupuncture. Researchers shined light on various parts of the body and found that light traveled under the skin to other acupuncture points, but it didn’t travel to places that were not on acupuncture meridians. It appears that the body contains a sort of fiber optic network—where light enters an acupuncture point, travels through the meridian and can be detected at other places along the meridian with a sensitive photon detector. This is a fascinating study showing how light is actually received, used and transmitted throughout the body.”
The RCT in question above is another paper by Raith W et al Laser Acupuncture for Neonatal Abstinence Syndrome: A Randomized Controlled Trial.
This study compared patients receiving treatment for NAS with morphine and phenobarbital and compared 14 in each group on a blinded fashion to laser acupuncture or nothing in addition to the standard regimen. They avoided the need for a placebo in that the intervention was done by the health care provider and then a separate person calculated a pain score who was blind to whether the laser had been provided or not. By blinding the people scoring they hoped to address the criticism that would be present had the study been unblinded. The acupuncture was performed daily at five ear and four body points bilaterally with the primary outcome being duration of oral opiate use. 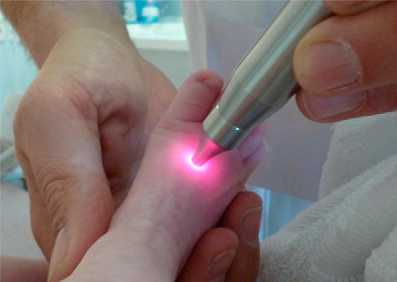 The authors found a reduction in days of opiate treatment but being a small study it would be considered a pilot at best. The results were 28 days (22 to 33) vs 39 days (32 to 48), respectively, P =.019 and the authors make a comment that phenobarb levels were similar between the groups as well but with overall shorter lengths of stay of 35 days (25 to 47) vs 50 days (36 to 56), respectively, P = .048. There are several issues with the study though and they are as follows. Yes, the light therapy was provided behind a closed door but how do we know that the providers truly kept it a secret during the whole stay of the patient? What medications were the mothers taking and at what doses and for what duration? Was the exposure between groups really the same? Also there was no standard means of weaning that I can see so how do we know by chance that the difference is simply who was on at the time with respect to physician deciding on aggressiveness of weaning. Another issue is that women on replacement medications such as methadone or suboxone were excluded as were women with polysubstance abuse. How close to our patient population really were these patients? Lastly, nearly significant was a preponderance of males in the conventional group and we all know how males generally do compared to females in most studies. Nonetheless it is a exciting study to imagine an effect from and that is what the authors I think were banking on.
The authors found a reduction in days of opiate treatment but being a small study it would be considered a pilot at best. The results were 28 days (22 to 33) vs 39 days (32 to 48), respectively, P =.019 and the authors make a comment that phenobarb levels were similar between the groups as well but with overall shorter lengths of stay of 35 days (25 to 47) vs 50 days (36 to 56), respectively, P = .048. There are several issues with the study though and they are as follows. Yes, the light therapy was provided behind a closed door but how do we know that the providers truly kept it a secret during the whole stay of the patient? What medications were the mothers taking and at what doses and for what duration? Was the exposure between groups really the same? Also there was no standard means of weaning that I can see so how do we know by chance that the difference is simply who was on at the time with respect to physician deciding on aggressiveness of weaning. Another issue is that women on replacement medications such as methadone or suboxone were excluded as were women with polysubstance abuse. How close to our patient population really were these patients? Lastly, nearly significant was a preponderance of males in the conventional group and we all know how males generally do compared to females in most studies. Nonetheless it is a exciting study to imagine an effect from and that is what the authors I think were banking on.
What about laser acupuncture for treatment of pain?
One other study comparing sucrose to laser acupuncture for prevention of pain with heel lances. In this study of 42 infants randomized to the intervention or sucrose the authors concluded that sucrose was superior to acupuncture for managing pain from heel lancing. This study did not have a third arm in which no treatment was given (likely due to it being unethical) so what we can’t say for sure is whether laser is better than nothing.
Personally I find a bit of a leap to believe that shining a light through the skin would have an effect on pain perception by anyone. I can certainly understand the concept of putting a needle into tissue or applying pressure no different from the effect of rubbing ones temples when they have a headache (works for me at least). The Chemistry major in me though has trouble with the effect of photons passing through tissue even if directed at acupuncture points. Having said that the only positive thing I can say is that a quick search for such instruments shows them to be commercially available and as cheap as $50 or so. I have no doubt there are people who will read this RCT and be impressed with its additional purported impact on NAS and thankfully if they do decide to pursue this intervention they will not have spent a fortune on it. Money in health care should be directed to what works to help patients and the skeptic in me just isn’t buying this even if it appeals to my curiosity with non-invasive strategies.

by All Things Neonatal | May 22, 2015 | NAS
In medical school you learn about the concepts of primordial, primary, secondary and tertiary prevention which can be explained in the following figure.
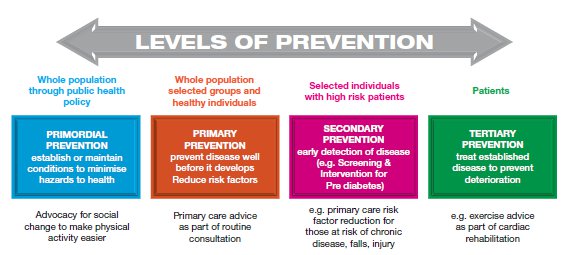
Simply put, from an impact standpoint you are far better to try to target the condition of interest with strategies to prevent the condition from happening than minimizing consequences once the condition is present in the patient.
As I wrote in another piece on Neonatal Abstinence recently we are experiencing an epidemic in mothers using opioids during pregnancy whether they be prescribed or obtained for recreational use. The US and Canada have taken great strides to enact preventative strategies to minimize exposure by introducing prescription tracking methods to monitor how often people are seeking these medications and identify those who are “doctor shopping”. While this should help deal with excessive use and furthermore curtail the selling to others who cannot be tracked, it still falls short of preventing people from using them in the first place.
We have the means to deal with the infants of these pregnancies but as mentioned in the other related piece, the number of hospital days and costs to the health care system have become staggering over time so clearly this is not the best option as we are focusing on tertiary prevention by treating the infants.
What inspired me to write this post was a publication entitled “Longitudinal cognitive development of children born to mothers with opioid and polysubstance abuse” by Nygaard E et al.
While long-term outcome studies on cocaine and alcohol as an example exist and show exposure in pregnancy can have both teratogenic and developmental affects, the impact of opioids in the long run has been less well-defined and limited to shorter lengths of outcome. An example of the effects of cocaine can be found here
Furthermore what is the impact of opioids in the presence of polysubstance use?
In the present study, the results are fairly alarming
Seventy two children with opioid and polysubstance exposure during fetal development were compared to 58 children without such exposure. Matching known risk factors for adverse outcome including such things as SES, placement in foster care was done. The results at 4 years showed similar results to other studies in that the groups exposed to the substances had lower cognitive functioning that the unexposed group with a mean difference of 10.5 IQ points at 4 years of age. What was striking though is that when the group was retested at 8.5 years of age, the gap had widened with a mean difference of 20.6 IQ points. Further analysis revealed that in fact the boys in the group had not deteriorated but it was the girls in this case that explained the difference with a mean difference of 14.4 IQ points.
The girls in this cohort showed substantial decline in cognitive abilities compared to the unexposed females.
This is the first study to show such cognitive decline over time especially in a female population. The reasons for this decline are speculative at best but may be related to different social functioning for females and males in foster care or other environments compared to males. Whatever the case, the exposure prenatally seems to have long-lasting consequences which become worse over time. In fairness I should mention that this is a small study and therefore open to risk of not representing what a larger cohort may show but the trend is certainly in keeping with other literature before it.
Coming back to the start of this piece, this publication serves as a strong reminder that if we wish to make a big difference to the greatest number of children we need to focus our efforts not on the problem in our NICUs but before the pregnancy occurs in the first place. Once the pregnancy has occurred public health campaigns could help educate women on the potential harm from using other substances when using opioids. An educational strategy is not doubt the way to go as the admission to the NICU is really the tip of the iceberg. The real cost is downstream and pertains to the societal impact, loss of function and dependency on the health care system for the rest of their lives. Lastly the children of these affected pregnancies themselves are at higher risk of repeating the cycle again enforcing the point that the time to do something is now using primordial and primary prevention.

by All Things Neonatal | Apr 27, 2015 | NAS
I work in an NICU that is no different in at least one way than yours. We have been seeing a growing volume of Neonatal Abstinence Syndrome (NAS) in our units for the last number of years. In fact I recall one week on service last year where 10/24 patients in our unit or roughly 42% were suffering from this condition. When I use the word suffering I should also mention that the staff experience this too. These infants are resource intensive in that they cannot be left alone for too long and as part of their management demand or require frequent feeding to keep their scores down.
Increasing Incidence of the Neonatal Abstinence Syndrome in U.S. describes the gravity of the problem in Neonatal ICUs in the US over the period 2004 – 2013.
As the saying goes misery loves company and the following graph tells the story of NAS in North America very well. There has been a dramatic rise in admissions with a progressive increase in length of stay. Attempts to curtail use of these drugs in pregnancy by criminalizing the use of drugs for the unborn fetus has not gone well; Mandatory Drug-Testing in Pregnancy: Lesson Learned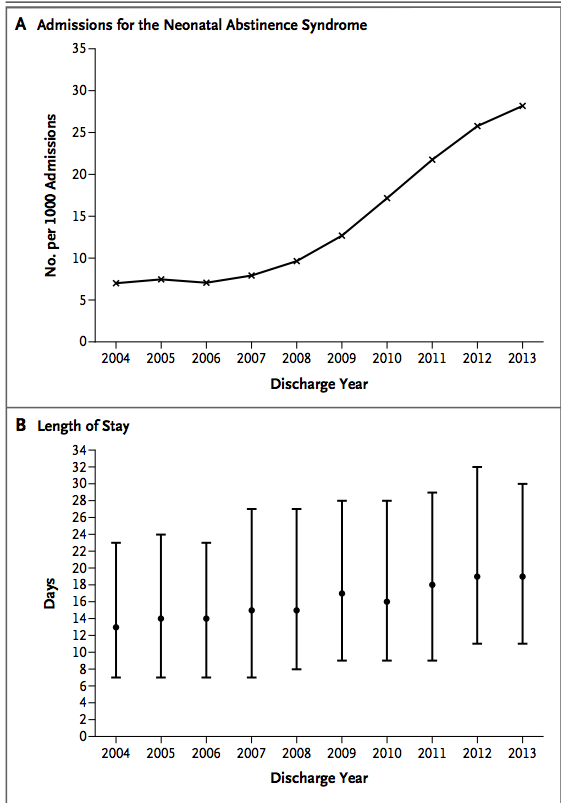
The use of opioid analgesic use in pregnancy has risen to an extremely high level and in large part is contributory in the US to such high rates of admission. The answer may also lie in a change to the approach of treatment that occurred in the middle of this epoch and is shown in the next figure indicating what type of medication was utilized for treatment. In 2010 the Cochrane Database for Systematic Reviews published a comparison of the evidence supporting either opiates or phenobarbital for the primary treatment of NAS.
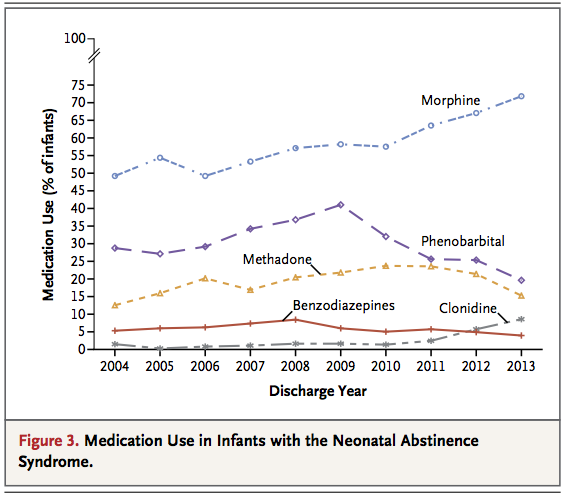
The conclusions of this paper changed the practice in our own and from the data presented here other centres as around 2009 – 2010, the use of phenobarbital decreased while morphine rose consistent with the recommendations from this group. Morphine was selected as it appeared to reduce the incidence of seizures although I have to mention I have never seen a case myself, so I remain curious as to how common they really are. In the review they also commented however that the use of opiates for treatment was associated with a prolongation of hospital stay. The reasons for this are in part explained by practitioner reluctance to discharge an infant home on an opiate. Doing so on low dose phenobarbital would have a much greater comfort level due to the common use for seizure control over the years in a home setting. This may be reflected in the findings as well in this paper that the practice of discharging on medications for NAS control decreased during the period studied from 4% down to 1-2%. Given the large number of babies being seen, this would represent a lot more infants in hospital and therefore a longer stay.
It is also tempting to blame the drugs that the mothers were exposed to but it would appear that there really is no basis for this based on this graph from the supplementary appendix The percentage of infants exposed to methadone remained the same, so higher use can not be blamed (which has been associated with higher rates of NAS).
Compounding the problem of NAS is that there are competing demands in many areas of the country where higher birth rates demand more NICU beds which are quite often occupied with NAS babies. There is clearly work that is needed in the field to turn the tide and reduce NAS admissions and certainly length of stay. As for how to do this there are a few ideas.
1. Might Burprenophine rather than methadone be a better option for maternal treatment? There may be something there
2. Treat the approach to NAS the same as that for headaches. Get on top of it quickly! Although not published, our own centre’s experience was that when we switched to predominantly using morphine we found that many of the infants required not only morphine but phenobarbital and often clonidine to control their symptoms and had the mean length of stay increase dramatically to 3-4 weeks per patient. What we discovered thanks to a very dedicated nurse with a passion for NAS management was that we were not doing what we said we would. Specifically, once the infant qualified for treatment we were not giving loads of 0.1 mg/kg of morphine q2h until controlled but rather in many instances waiting a little longer and then using 0.05 mg/kg as loads. Since reinforcing that we need to get on top of the issue right away (like with a headache before it becomes entrenched) the use of morphine monotherapy has increased dramatically.
3. Never admit these children in the first place. We have an agreement with the postpartum ward that the initial monitoring for NAS can occur in the room with the parents. The lack of separation encourages breastfeeding which in and of itself has led to some infants being successfully managed without ever coming to the NICU. We still see infants coming but those that do have had 2 -5 days less time in the NICU decreasing the usage of NICU beds for this purpose with the added benefit of increasing maternal/infant bonding. Better yet there are models out there of mother-infant homes that these dyads can be discharged from hospital to. Having them out of the hospital environment may be the best thing for them altogether and avoid treatment with medications at all.
4. Consider discharging infants on morphine or other opiate. There is no question that during the acute phase these children need to be in hospital as there are significant side effects from morphine not the least of which is respiratory depression. Once a patient in weaning from the morphine and has successfully decreased the dosing or interval by 30 – 50% it is exceedingly unlikely that on the lower daily dosage they will start having symptoms. In the presence of a reliable family with good supports that has been screened by a social worker such treatment can be completed outside the hospital. Some may be worried about what could happen if the medication is taken by an older child or parent but as you know the amount of drug that would be sent home when dosed at 0.05 mg/kg or less for a few doses would not impact such larger individuals.
I am grateful to NEJM for publishing this article as it shows we are not alone. Your suspicions that NAS is on the rise are accurate. NAS is here and it’s not going anywhere. The question is what are you going to do about it?!

 This post is very timely as the CPS Fetus and Newborn committee has just released a new practice point:
This post is very timely as the CPS Fetus and Newborn committee has just released a new practice point:





 Aside from the societal issues these families face and the problems their infants experience, the swelling volume of patients NICUs have to contend with are quite simply overwhelming resources with time. Although I reside in Canada, it is the trend shown that likely motivated some states to adopt such a draconian approach to these mother-infant dyads.
Aside from the societal issues these families face and the problems their infants experience, the swelling volume of patients NICUs have to contend with are quite simply overwhelming resources with time. Although I reside in Canada, it is the trend shown that likely motivated some states to adopt such a draconian approach to these mother-infant dyads. where a mother could conceivably take a medication that she is unaware is on a list of “banned substances”. What about Naturopathic or herbal supplements that might test positive?
where a mother could conceivably take a medication that she is unaware is on a list of “banned substances”. What about Naturopathic or herbal supplements that might test positive?





