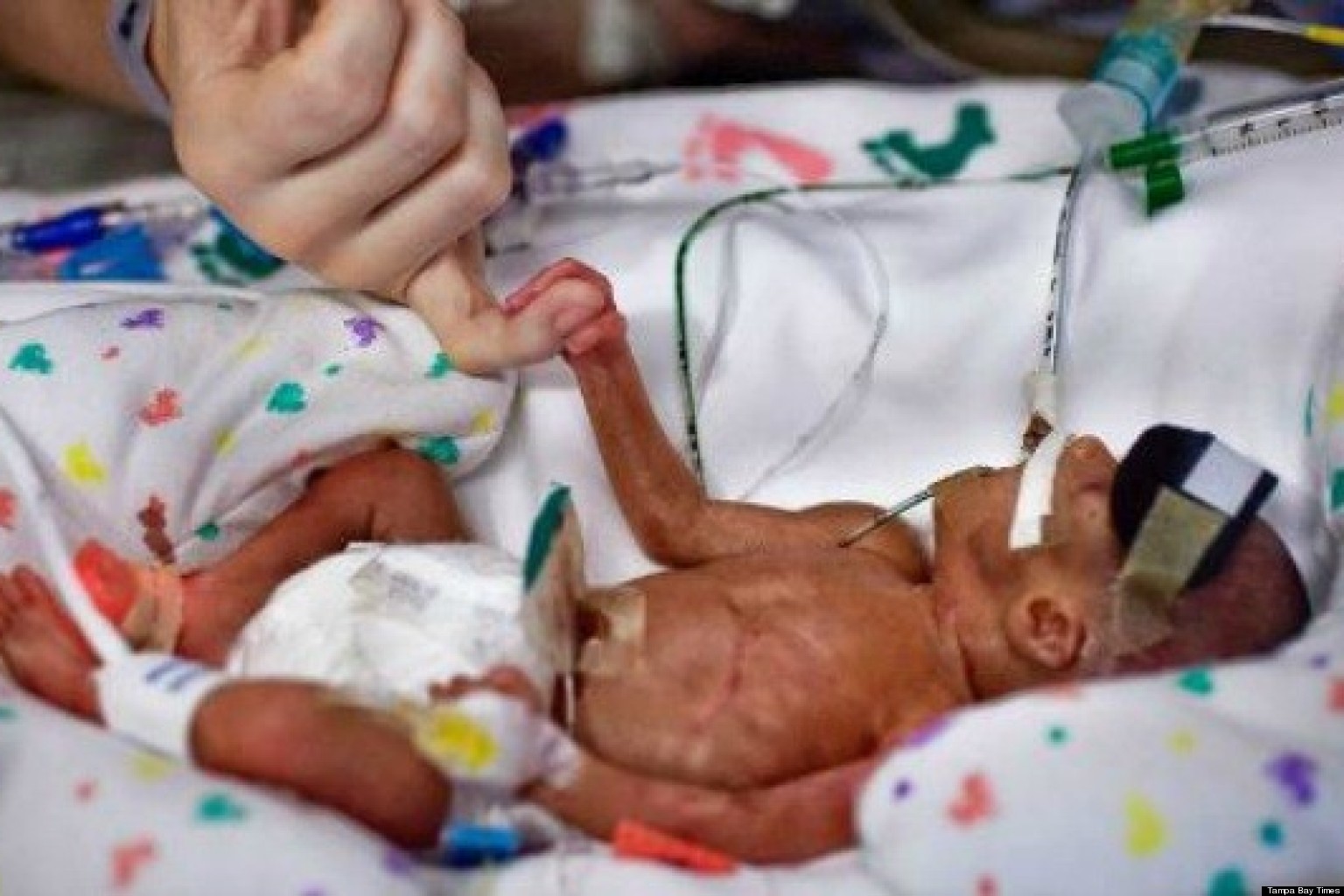
by All Things Neonatal | Sep 21, 2016 | bioethics, preemie
While we draw the line at 22 5/7 weeks for offering active resuscitation where I work, what does one do when the family requests resuscitation prior to that point. While I am a clear fan of social media, one consequence of having such widely available information at our fingertips is that families may already know before you come to speak with them that were they only to have been born in another place like Montreal, the cutoff would have been lower. When faced with such demands what does one do? Well, in the case of my own experience it was to give in to the demands of the parents. While I certainly discourage such heroic attempts, what is one to say when the family having received your opinion states “I want everything done”. Informed consent is a tricky one in that if you approach a family for informed consent and they refuse to accept your desired direction of care where does that leave you? It leaves you with informed refusal and if we are being fair to our families we have to accept that informed refusal is just as important as informed consent.
Nothing New?
The truth is informed refusal has been recognized as being critically important to decisions in patient care for many years. Previous papers on the subject include a nice review by Ridley DT, Informed consent, informed refusal, informed choice–what is it that makes a patient’s medical treatment decisions informed? What this really comes down to is a patient’s right to personal autonomy and self determination. Does a parent in this case have the right to do what they want even in the face of dismal odds? Furthermore where are we placing the importance of values? Is it physician or patient centric? In the physician centric world, after we impart our experience and wisdom we expect the patient to generally follow through with what we are steering them towards in cases such as this. Informed consent of course is meant to be free of coercion but let’s face it, when we truly believe something is fairly futile are we honestly playing an impartial role or using our tone, body language and choice of words to direct families down the path that fits with our own beliefs and values? I would offer that in most cases when we seek informed consent what we are really doing is seeking to pass along the justification for what we are wanting to do and then moving forward once obtained.
What do we do though when after hearing the pros and cons the family still opts to move forward and worse yet is in disagreement with our preferred plan. Well there you arrive at informed refusal. If after hearing our best transfer of information the family still wants to proceed what does one do? As a physician if I believe something is completely futile and I find myself in this position then I am truly at fault. Seeking informed consent in this situation was completely inappropriate. One should have simply said there is nothing that can be done.
The Montreal Example
Getting back to the example that started this piece, if a family knows that there are places in Canada (or let’s be honest, if I know there are survivors in Canada at 22 weeks) that resuscitate and have survivors then it isn’t really futile is it. I know many of you would say “but the odds are so stacked against the baby” and “they don’t know what they are getting themselves into” but what does one say in this circumstance when despite your best attempts the family still wants to resuscitate?
Therein lies the challenge. If we approach this as an opportunity for informed consent we need to accept that we may find ourselves face to face with “informed refusal”. Now I need to be careful here. I am not advocating a wide open optimistic approach to resuscitation at 22 weeks. What I am suggesting though is that if you find yourself coming into a unit somewhere in the next few months and find yourselves looking at a 22 week infant don’t jump to conclusions! Did the family despite all the warnings want this? Don’t leap to the thought that the Neonatologist is pushing for this but rather it may indeed be a case of a family advocating for their child against all odds. It may not be something that we agree with in many cases but are we thinking from the perspective of the family or our own value system?

by All Things Neonatal | Jul 1, 2015 | bioethics, LGBT, Neonatal
This is a lengthier piece than normal but the message at the end is critical to disseminate so I would encourage you to share this if you wish with others to prevent misinformation from being propagated in the media by the sensationalism of a claim by a group of Pediatricians.
My Facebook page became awash in rainbow overlaid posts on Friday. Very quickly I realized as did most of the developed world, that the US Supreme Court ruled in favour of same-sex marriage and just so no one thinks that this will turn into a homophobic piece, I celebrated the change along with many friends and fellow Social Media colleagues.
After the initial excitement began to wane I came across a press release that I found a little shocking given that I belong to the group of people (as a Pediatrician not a member of the organization) that released the statement shown below. The statement is from the American College of Pediatricians
by ADMIN3 on JUNE 27, 2015 in PRESS RELEASE
Dr. Michelle Cretella, President of the American College of Pediatricians in response to the SCOTUS decision today stated, “[T]his is a tragic day for America’s children. The SCOTUS has just undermined the single greatest pro-child institution in the history of mankind: the natural family. Just as it did in the joint Roe v Wade and Doe v Bolton decisions, the SCOTUS has elevated and enshrined the wants of adults over the needs of children.“
Although it is disappointing only 4 of the 9 justices heeded the scientific findings in the
College Brief, the College will continue to proclaim the important unique contributions of both mothers and fathers to the optimal nurturing of all children.
As I went to their website and read about this organization it became clear that this group is mixing Church and State so to speak. Their mission statement states:
Mission of the College
The Mission of the American College of Pediatricians is to enable all children to reach their optimal physical and emotional health and well-being. To this end, we recognize the basic father-mother family unit, within the context of marriage, to be the optimal setting for childhood development, but pledge our support to all children, regardless of their circumstances.
Who are these people and why are they speaking out in such contrast to the American Academy of Pediatrics who in 2013 published their technical report in support of same-sex couple raising children. The AAP which has about 64000 members dwarfs the membership of possibly 200 Pediatricians that comprise the American College of Pediatricians. The smaller group was formed when a group of Pediatricians became upset in 2002 of the AAPs position that endorsed same-sex couples adopting children. The trouble of course with an organization such as this is that their name implies some degree of credibility but in looking at their track record on this issue they have little to none. They are a group that seems to ignore the literature discussed below in favour of quasi-scientific religious literature suggesting harm from such family units. The support of the AAP, the dominant organization in the field was made clear June 26th with this statement. I particularly like the quote from the president of the AAP.
“Every child needs stable, nurturing relationships to thrive, and marriage is one way to support and recognize those relationships,” said Sandra G. Hassink, MD, FAAP, AAP president. “Today’s historic decision by the U.S. Supreme Court supports children in families with same-gender parents. If a child has two loving and capable parents who choose to create a permanent bond, it’s in the best interest of their children that legal institutions allow them to do so.”
Putting aside my natural suspicion of the American College of Pediatricians, it did lead me to ask an important question. Are kids truly better off being raised in a heterosexual marriage? Perhaps there is evidence to show that indeed this is something that we as Pediatricians should be promoting. Looking at the evidence though would suggest otherwise or at least that there is no difference. In 2014 the largest study to date was published by Australian researcher Crouch et al involving 315 parents representing 500 children from same-sex marriages (complete study here). The study involved a questionnaire that would then be compared against population data to see if differences exist between parental units. A little over two-thirds of the parental units were Lesbian. The results demonstrated that in virtually all measures of child health the parental units were equivalent. Curiously, sense of stronger family cohesion was present with the same-sex groups. Possible reasons for this may be related to the way in which children are brought into this world in the two parental unit types. Given that people of the same-sex must plan (there are exceptions no doubt) to procreate there is little chance of the unexpected pregnancy occurring. These are almost all “wanted or chosen” children as opposed to the situation encountered in many pregnancies that are not planned. That is not to say that these children can’t or won’t be loved but the likelihood seems much lower in a LGBT parenting situation due to the planning that is generally required. While the research did not go on to elaborate on why the cohesion might be enhanced this is just my speculation.
Adding to this piece of evidence that these children are likely to have equivalent health to the traditional family rearing model is a well-timed report that surfaced the same week as the Supreme Court Ruling. The report from the Huffington Post challenges that after reviewing 19000 studies on same-sex parenting there can be no conclusion that the children of such families are worse off in any measure of health. Where the above group derives their mission statement from then is certainly not based on science but rather perception.
Back to the American College of Pediatricians (ACOP). I mentioned earlier that I was suspicious of the ACOP and what they portray as advocating for a child’s best health. As a writer of a blog I firmly believe that the buck stops at me with respect to content. If I have a guest writer I am responsible for their content as well as my own. I took the liberty of reviewing a recent piece from their blog and what I saw both shocked me and left me with the certainty that this group is not so much advocating for the health of children as condemning those lifestyles that they do not believe fit the mother-father mold. On June 5th the group released the following piece entitled “P” is for Pedophile. Please click on the link if you have the stomach for it but to give you a taste of what they are talking about here is the quote from the first line of the entry.
“Driving in this morning I began to wonder. Why isn’t the movement of LGBT not the PGBT movement: “P” for pedophile?”
If this group had any credibility by having a professional sounding name, my hope is that this post will spread wide and far to help discredit this organization. The evidence suggests that members of the LGBT community raise just as healthy kids as any of us and any attempts to smear people simply for who they happen to bond with for life amounts to hate and there should be no room in Pediatrics or any other field of medicine for that.

by All Things Neonatal | Jun 20, 2015 | bioethics, Neonatology
I was asked to see a woman carrying a fetus this week who was not yet 21 weeks. It was to be honest a very unusual consult as she was clearly pre-viable to me and this was only the second time in my career that I had been asked to do so before 22 or 23 weeks. In the course of our conversation she said the following:
“I know I just have to get to 22 weeks. Everyone knows that at St. Boniface Hospital they are saving kids at 22 weeks now and they will try to resuscitate mine if I can just get a little longer out of this pregnancy”
You might think I was shocked to hear this but I wasn’t as I had warned a group of health professionals ironically minutes earlier that we were going to start hearing things like this due to misinterpretations of both the medical literature and mainstream media. When I asked her where she heard this, her response was that everyone at the clinic she goes to are talking about it. I can only wonder how many other clinics, mom’s groups, Twitter and Facebook posts are saying the same thing! I spent some time with her and provided her with my view on the topic and we agreed not to do anything for her infant until they were bigger (currently was under 300g) and at least 22 5/7 weeks. I am not saying I necessarily believe we should strongly go for an infant at 22 5/7 weeks but she is right that we have and if taking in all the information she wants us to try, now that the public is aware how can we not?
Before I go on let me be clear about the actual state in our city at the moment:
WE ARE NOT RECOMMENDING RESUSCITATION OF ALL INFANTS AT 22 WEEKS OR EVEN 23 WEEKS BUT ARE HAVING DISCUSSIONS ABOUT 23 WEEKS
One Article Causes A Great Stir
In late April the New England Journal of Medicine published an article entitled Between-Hospital Variation in Treatment and Outcomes in Extremely Preterm Infants. What followed were numerous media articles about infants born at 22 or 23 weeks discussing the pros and cons of such actions. Furthermore an explosion of testimonies from parents who had infants resuscitated with good outcomes at these gestational ages ensued. Given that this topic was a hot one and in the public eye, our own local health news agency got in on the action and published the following story called Meet Mac: one of the youngest babies born at St. Boniface Hospital which was reprinted by the Free Press thereby achieving a larger audience.
The family is wonderful, the child simply amazing and much like many of the aforementioned similar stories on Facebook and Twitter inspires people to have hope. We all want in the end to feel good about things rather than dwell in sorrow so when these stories come along we tend to see them in a favourable light rather than critically analyze what they mean in the context of the greater picture. In the article they reference, such children as miracle babies and in many respects this is true. Before I go on I feel the need to point out that I am delighted for Mac’s family and admire their perseverance through many dark days. There is no question that they are a loving family who will love him for the rest of his life and provide a wonderful nurturing environment. The concern I have is that they are in the 5% or less of families that have this experience.
If we look at the article referenced above from the United States which is the largest study to date looking at extremely low birth weight infants the findings were that 95% of those infants who people tried to resuscitate at 22 weeks either died or were left with moderate to severe disabilities. This means 5% survive with only mild or no disability. It is the 5% we tend to hear about in the media and are the ones that create the buzz.
Looking For National Guidance
The fly in the ointment in all of this is that the Canadian Pediatric Society that provides recommendations in such situations is also under fire for its statement on Counselling and Management of Extremely Preterm Birth. In this statement in the recommendations section they state: At 22 weeks’ GA, since survival is uncommon, a non-interventional approach is recommended with focus on comfort care. (Strong Recommendation). In response to this statement a great number of practitioners banded together to write a rebuttal that was published in Pediatrics and Child Health in which they believe that the CPS has created simple rules for complicated decisions as the title of the article suggests. The gist of the article is that gestational age alone is inaccurate and using other prognostic factors in addition to gestational age is a better way of guiding decisions. Factors such as estimated weight and certainty of dates for example should come into the picture. Time will tell how the CPS responds but certainly organizations such as the Canadian Premature Babies Foundation are siding with the authors of the response to the CPS.
Make no mistake, this is a complicated issue and it will not go away anytime soon. While we are not advocating for 22 week infants to be resuscitated routinely, the fact remains if well informed parents decide they want to try it will be difficult to say no. Parents need to understand however that for infants to have the best chance, a coordinated approach with Obstetrics and Neonatology is critical to ensure the best chances. Furthermore seeking the opinion of a Bioethicist would help crystallize some of the issues that I know many are struggling with. Failure to receive antenatal steroids at 22 or 23 weeks for example is clearly shown in this article to reduce the likelihood of a positive outcome. Having a face to face discussion between the Neonatologist and Obstetrician and presenting a unified message to the family will be an imperative first step in any discussion. Furthermore having clear direction in a resuscitation and best practices worked out in the NICU to ensure that skin integrity is maintained is a must. We have a long road ahead of us before we can truly say that we are offering the best chances to these tiny infants but with collaborative efforts between our members in Neonatology and Obstetrics I believe we can get there.
In the meantime we each need to do our part and use our voices (or writing such as this) send a clear message to the public that while we celebrate with the families who have had such great outcomes at these gestational ages we all too often are mourning the loss of the vast majority who were not so fortunate.
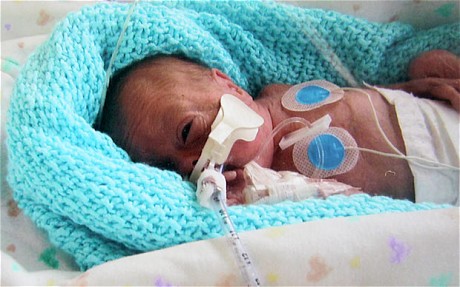
by All Things Neonatal | Jun 11, 2015 | bioethics, Prematurity
A judge has granted a man the right to a physician assisted death in Manitoba as reported by the CBC yesterday. Given this landmark ruling based on a change in the Canadian stance allowing such decisions the question turns to children and then neonates. At the present time this stance does not apply to these populations but it is fair to ask the question… what if it did?
The Groningen Experience
As the saying goes “the more things change the more they stay the same”. In 2005 I was but a year into my career as a staff Neonatologist and we were discussing whether we should resuscitate 22 and 23 week infants. Sound familiar? In the back and forth discussion, one of the things that came up from time to time was that the Dutch at least had the option of euthanasia to fall back on if they decided to resuscitate an infant and then the family or care providers changed their minds. It was not necessary to prolong the suffering of the family and patient in the face of futility. I remember being shocked by such a ruling in Holland’s legal system, as euthanizing a newborn in North America was and still is today something that most could not come to grips with. Nonetheless the Groningen protocol as it became known, was introduced in 2004 by Eduard Verhagen the medical director of the department of Pediatrics at the University Medical Center Groningen and became endorsed almost 10 years ago to the day by the Dutch Society of pediatrics.
Although many of you may be caught off guard as you read this, it really did generate a fair bit of attention here in North America and has been the subject of many articles and news reports over the years. The Groningen protocol is quite extensive as shown in the table.
The key elements to the protocol are: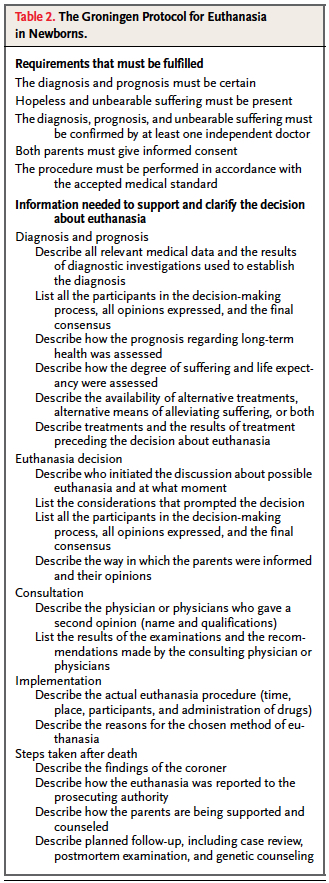 
(1) diagnosis and prognosis must be certain
(2) hopeless andunbearable suffering must be present
(3) a confirming second opinion by an independent doctor
(4) both parents give informed consent
(5) the procedure must be performed carefully, in accordance with medical standards.
There were some that worried birth at 22 weeks would meet this criteria and lead to ELBW infants being euthanized after a few hours of life rather than using the method of comfort care that we are accustomed to in North America if carrying on seemed futile. Although the outcome is the same, the route to get there is clearly different.
So the question then is what has happened in Holland since this practice was made permissible by the courts? In 2005 shortly after the protocol was introduced, Verhagen published a piece in the NEJM reviewing all the cases of newborn euthanasia from 1997 – 2004. In all there were 22 cases each of which involved a case of spina bifida and in most quite severe. Interestingly there were no cases of premature infants.
What Happened in Holland Over Time
In 2013 he published a a second article in which he acknowledged that worldwide people were concerned that a slippery slope would occur in Holland. As such, he examined all neonatal deaths in NICU from 2005 – 2010. Withholding or withdrawing treatment was the reason for death in 95% of cases. During that period only 1 patient with Osteogenesis Imperfecta type II was classified as euthanasia. This dramatic decline from the pre 2005 state may seem surprising but it is offset by an increase in second trimester terminations after ultrasound at 20 weeks became standard practice in Holland. Previously it was only offered to those over 35 years of age. In fairness, he does acknowledge that there could be underreporting occurring but as he points out, given the lack of consequence in the legal system provided that the protocol is followed there would be little reason to not report as such. There are some cases of paralytic use described in what was classified as withdrawal of support in which the medication was used to treat the gasping efforts of the infant in the last moments of life. While these cases are technically euthanasia, in that the end of life is no doubt hastened, at that point it could be measured in minutes. Is that so wrong if the team views this as distressing to the patient and family. Perhaps yes in some eyes but ask yourself if it is that different from knowingly pushing doses of narcotics higher in the same circumstance which achieves the same end point at times.
So it would seem that the rate did not increase and in fact a marked decrease actually occurred. Curiously a second study has been just released Dutch neonatologists have adopted a more interventionist approach to neonatal care. The study is a joint effort by the Dutch including Verhagen and Dr. Janvier of St. Justine in Montreal who we were fortunate to hear speak recently in Winnipeg. The paper describes a very interesting phenomenon. The authors compared all infants born at > 22 weeks who either died in the delivery room or in the NICU in two epochs; 2001 – 2003 and 2008 – 2010 specifically looking at measures of intervention in the two periods. Would more legal clarity making it permissible to end a life lead to higher mortality in the second period, as a marker of less invasiveness? In both periods there was only one patient that received comfort medication in the delivery room. Furthermore, there were no differences in the number of patients dying in either site. As described in the 2013 paper there were increases in the rate of termination of pregnancy in the second period but there is no support for the argument that the Dutch became less interventionist after the relaxing of laws on euthanasia. Lastly as further evidence that they went the other way, length of stay increased significantly in the NICU from 11.5 to 18.4 days in the second period reflecting less withdrawal in part.
What Conclusions Can We Draw About Our Own Populations?
As the title of this post suggests, it would appear that much of the worry in 2005 has simply not come to pass. Yes there has been a shift to termination for congenital anomalies in the second trimester but that would be no different from our practice in North America. I can’t help but draw parallels between the arguments for the legalization of some drugs such as marijuana and euthanasia. The decriminalization of the former is expected to have the benefit of reducing crime and perhaps even abuse of the drug as it no longer becomes as attractive once it is no longer “sinful”. Has a similar effect happened in Holland perhaps by bringing the discussion to the world stage? It may well be that the change in law in Holland created the opposite effect whereby the Dutch painfully aware that they were being “watched” became even more reluctant to hasten the time of death in these situations. There is no doubt that something changed after 2005 as they became more interventionist and not less.
A final thought has to do with a thought that Dr. Verhagen raises in the 2013 piece. Has the transition to a model of terminating pregnancies in the second trimester been a good or bad thing. He argues that ultrasound is not as predictive in terms of diagnosis as examining a patient after birth. When an infant is in front of your eyes, facial features combined with enhanced imaging may reveal a change in diagnosis compared to what is determined antenatally. Similarly, a patient with a seemingly inoperable heart defect may have a slightly different scan after delivery which provides some options for the family. If examination after birth is superior to antenatal diagnosis in terms of accuracy, are we doing the right thing by forcing families to decide on termination prior to delivery? In Holland the option exists although clearly not being taken to assess a patient after birth and then if the diagnosis meets the Groningen protocol a life can be ended early. It can be argued of course that euthanasia is not the only option and that one can choose not to feed and withdraw life-sustaining treatment.
The question that I will leave you with though is as a parent would you want to watch your infant die after 5-7 days dehydration or end their life given the outcome is the same on the same day you choose “compassionate care”? Which is the more humane decision when the outcome is the same?
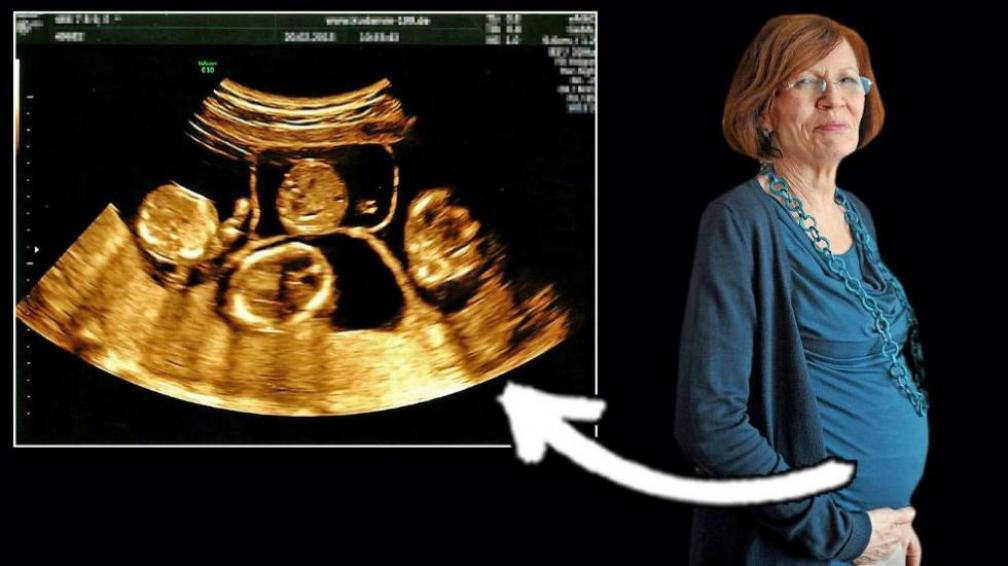
by All Things Neonatal | May 30, 2015 | bioethics, Neonatal, Pregnancy
A couple months ago on my Facebook Page (www.facebook.com/AllThingsNeonatal) I posted the shocking story of a 65 Grandmother Annegret Raunigk who received IVF and was carrying quadruplets. The post spawned outrage among my followers with statements that it was simply wrong while others argued that the risks of the mother giving birth to premature infants who would need extensive support was extremely high and that it was unethical to have done so. From my standpoint I agreed with the comments and so here you have it; the mother (or grandmother) has given birth.
http://www.cnn.com/2015/05/24/europe/germany-grandmother-quadruplets/index.html
She has delivered four premature infants < 26 weeks gestational age. Assuming they are 25 weeks each the outcomes for these babies may not be as dire as one might think. We would expect for singletons about a 70 – 80% survival with about 50% surviving without moderate or severe impairment. With quadruplets I would expect lower numbers so the reality is that at least two of these kids will have significant health care needs in the future. I would ask that we leave aside the arguments that may ensue at this point by bioethical purists who may argue that the babies’ perception of their quality of life in adolescence would be better that ours. The reality is that even if this were so, this single mother has now given birth to 17 children of which her last four are extremely low birth weight.
Who will be there to care for these children? What about the impact on society? in the next ten years will she have the energy to provide the stimulation, take the kids to all their appointments and so forth that will be needed to ensure an optimal outcome for them from a developmental standpoint?!
This is wrong on so many levels and it is not enough to say as they mention in the article that doctors encouraged her to undergo fetal reduction by one or two fetuses at an early stage. That excuses the IVF treatment in the first place by ignoring the fact that the opportunity to do something about this was missed at the first doctor’s appointment when she asked for the IVF treatment.
Nadya Suleman the “Octomom” give birth to eight premature infants and became known the world over in a sensational news story that followed her through her pregnancy and birth. It is another example of the medical community embarking on a path that lacks responsibility and ignores one of the founding principals of our Hippocratic Oath “To do no harm”. Nadya’s physician in her case suffered one of the most appropriate punishments that California could dole out. He lost his license (http://nydn.us/1d5rSxc), she went on to file bankruptcy, spoke out against the kids she wanted so much and finally resorted to pornography to pay the bills (http://huff.to/1AE5HsR). I can only wonder if the mainstream media’s obsession with Nadya’s story sparked desires for copycat sensational pregnancy stories elsewhere. Annegret Raunigk will not doubt receive a tremendous amount of attention as she already has so is there another agenda over and above to have children that is at work here?
As a medical practitioner it is generally ill advised by the local Colleges to speak out publicly against another physician but in this case this doctor who chose to implant embryos into the 65 year old mother should suffer the same fate and lose his license before he does such a thing again. He lacked judgement and any sensibility in creating a situation that would almost certainly lead to four extremely premature infants being born. I hope the German medical community acts to remove such a physician (I use the term lightly) before he can cause any further damage.
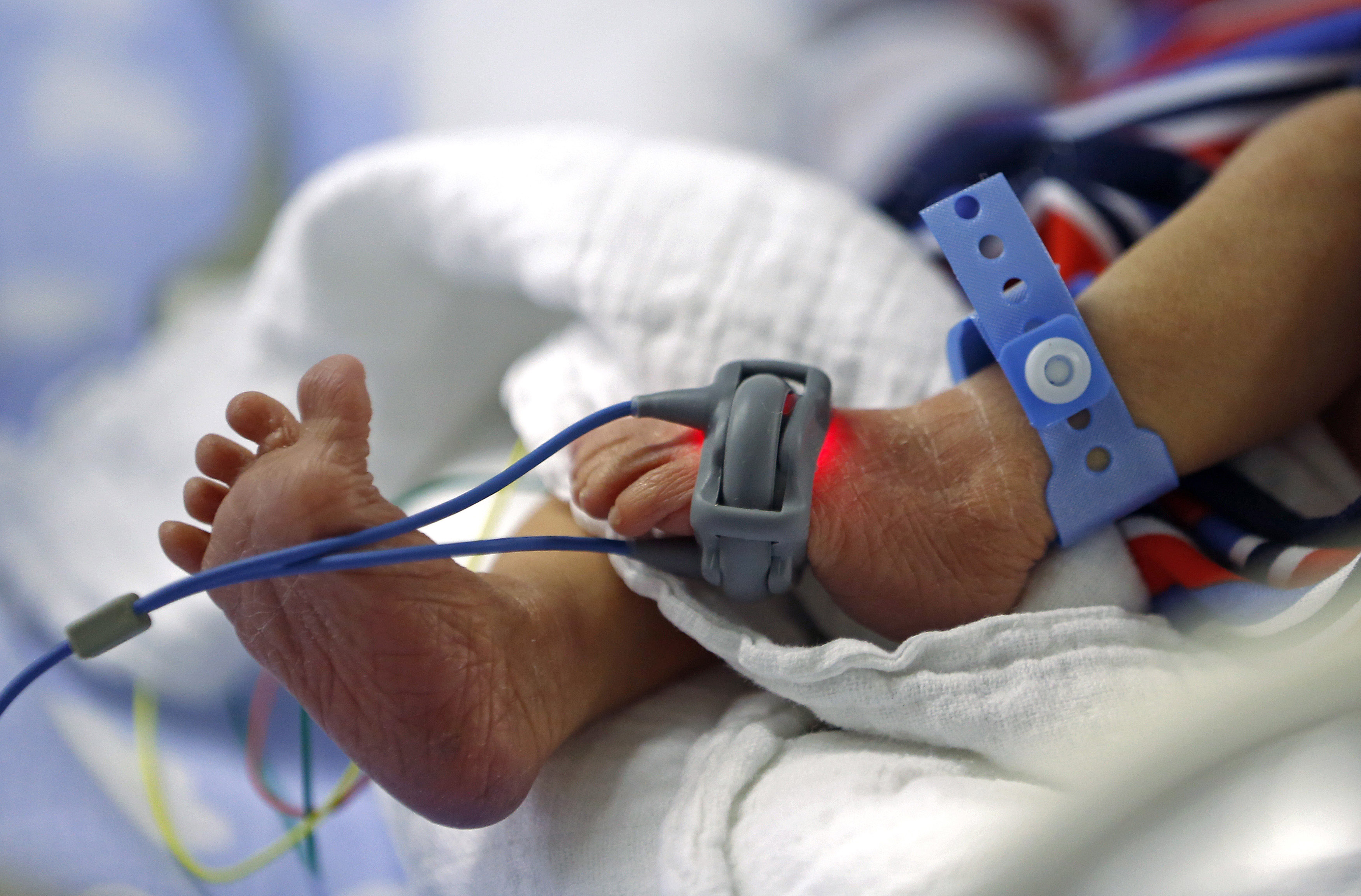
by All Things Neonatal | May 25, 2015 | bioethics, Neonatology
Virtually every popular media site and especially those dedicated to covering the world of Obstetrics and Neonatology have been ablaze with discussions on the NEJM paper Between-Hospital Variation in Treatment and Outcomes in Extremely Preterm Infants. Since this publication, numerous blogging sites have similarly expanded on the coverage with testimonials of success stories of infants born too small or too young who survived and in most cases nearly intact.
Other posts are even more sensational, claiming that the infants have done extremely well and are in fact normal and healthy. The stories capture all of our attention and as feel good pieces give us pause to reflect on the tenacity of our beliefs either for or against resuscitation of these patients. Even more powerful are those instances when our health care teams experience a good outcome at these gestational ages. These types of cases challenge even the most ardent individuals that as a rule we should not intervene before 24 weeks.
How Likely Is A Good Outcome at 22 & 23 weeks?
What we have to remember though is that at least for the 22 week infants < 10% of those reported in the US cohort survived without moderate or severe disability and in the case of the 23 week infants these numbers although better, gave a 1/6 chance of surviving without that outcome. Flipping this number on its head to present a glass is half empty argument, there is a 5/6 or an 83% chance that a child born at 23 weeks who is actively resuscitated will either die or be left with a moderate or severe disability. The blog posts from this group of parents are far less common, although I have no doubt many of these parents were happy they at least tried. Had they not they would have been left wondering for the rest of their lives “what if”?
The purpose of this post is not to debate the rightness or wrongness of the desire to resuscitate or not. Rather I would like to discuss the fallacy of thinking that informed consent plays any role in most of these cases. All too often clinicians hide behind the veil of “informed consent” as justification for the family choosing to move forward with the decision to try to resuscitate these small infants. Is that what is really happening though in most cases? Sadly, in the nearly 12 years I have been in practice in these circumstances I suspect the conditions for true informed consent have been absent more often than not. Yet the Canadian Pediatric Society lists as the third recommendation in the statement “Counselling and management for anticipated extremely preterm birth”
“Decision making between parents and health professionals should be an informed and shared process. Decision aids may be helpful for parents. (Strong Recommendation)”
The issue lies in the criteria to obtain informed consent.
The Merriam-Webster Dictionary provides this definition:
“A formal agreement that a patient signs to give permission for a medical procedure (such as surgery) after having been told about the risks, benefits, etc.”
Unless a family has previous experience with a baby born at 23 or 24 weeks (outcomes after that become quite different), or they themselves work in the field of Pediatrics and have seen the range of outcomes that these children experience, how can they really know what the risks and benefits are?
As a young medical student I recall being told time and time again to be careful about the use of medical jargon. Rather, ensure that you use lay terminology that the parents can understand, in order to ensure that informed consent can be obtained or that the family understands the clinical course of their child. How many times have I talked to families using such words of wisdom only to think in the back of my mind; “do they really understand what I am saying?”.
What do they know of chronic lung disease, PDA, IVH, ROP and a host of other problems? What can they possibly know what their lives will be like in 2, 5 or 10 years down the road should their infant survive but with a host of major medical issues? Add to this, that in many cases there is little time for discussion as the mother presents with rupture of the membranes and goes on to deliver within 48 hours of presentation and often an even shorter time frame. Furthermore, the history of the pregnancy can be extremely motivational in helping a family decide what course is right for them. How does the mother who has had three rounds of IVF perceive the situation compared to the 16 year old who had an unplanned pregnancy. Clearly the psychological factors at play must have a tremendous influence on the decision.
Many parents are simply not in a state to receive the information even if it is presented well.
A study by Boss R et al suggests that what we say has very little impact on the parental decisions (Values parents apply to decision-making regarding delivery room resuscitation for high-risk newborns). In this paper, 26 mothers responded to a questionnaire at a minimum of 10 months after the death of their infant who was born between 22 and 25 weeks. After being asked about the discussions they had with their Neonatologist and Obstetricians these were the four main points uncovered.
1. Parents rarely perceive that there are options for delivery room resuscitation. They recall being told information but rarely that compassionate care was even an option even if this was documented in the chart.
2. Physicians’s predictions of morbidity and death are not central to parental decision-making regarding delivery room resuscitation. In essence the parent’s “gut instinct” which was nearly uniformly positive guided their decision.
3. Religion spirituality and hope are the primary values that parents apply to decision-making regarding delivery room resuscitation.
4. Parents feel abandoned without physician hope and compassion. There was mistrust of doctors who only emphasized the negative without a sense of emotion. Relaying the facts is not enough.
When under such stress is it possible for families to weigh all of the true risks and benefits and come to a conclusion that satisfies the requirements for informed consent? Given that to do so requires that an individual be in a state that allows them to process this information and take their time in coming to a conclusion I think in most cases the answer is no.
Planning a Path Forward
If your centre is planning to cross over the threshold of 24 weeks there must be a coordinated plan between the delivering obstetrician, neonatal team and family. Most parents are in no position to truly appreciate what we are telling them either because of the emotional frightened state they are in or because the overpowering urge to “do everything you can” takes a front and centre position in their mind. All we can do as the Health Care providers is to provide them with as accurate information as we can and support each family after they make their decision. Once that decision is made we must also realize that once we embark on a path it is not permanent. If the condition of the newborn is such that survival without severe disability becomes increasingly unlikely we owe it to the whole team (including the family at the centre) to revisit what would be the best course of action.







