How important is chronic lung disease anyway?
It is interesting to look in the rear view mirror. This post was the first ever on All Things Neonatal. Was it predictive of something to come with respect to the way we look at BPD? I think the followup post to this on this site gives that answer “The New BPD That Matters“. BPD is not what it once was and how we characterize infants with BPD is in need of change. What do you think?
Shah and others from the Canadian Neonatal Network published the following paper recently in The Journal of Perinatology. Association of unit size, resource utilizaton and occupancy with outcomes of preterm infants. The paper examines the relationship between the factors in the title and the composite outcome of all mortality plus a basket of severe adverse outcomes including severe IVH, BPD, PVL, NEC and others.
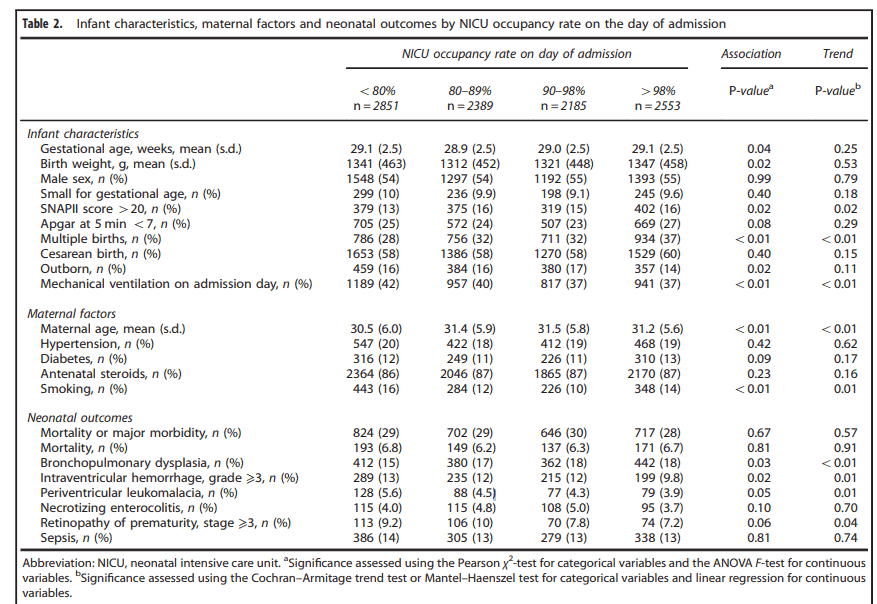
In the end it is the finding of more intense resource utilization at admission rather than size of the unit that seems to make the biggest difference to outcome. Larger units do not fare any worse than smaller although it is a curious finding as one might expect that with more experience comes better outcomes. As this study can only show an association the analysis may be limited in terms of take home points.
What we can do with this information is where the interesting part comes for me. Sicker babies that need more resources at admission have worse outcomes. Would increasing nursing levels, physicians caring for these children, equipment purchases etc make a difference? I don’t know as it may simply be that the infant’s outcome is determined by the acuity rather than having sufficient resources to avoid spreading your workforce too thinly. Perhaps further research will tell us if what we believe would intuitively help will actually make a difference.
The other point in the article that I find intriguing and have for a long time is the way the CNN (Canadian Neonatal Network) handles BPD. It is not just O2 supplementation at 36 weeks which determines the diagnosis but also if O2 is being used at transfer to a level II nursery. How can one label a baby at 32 weeks as having BPD to the same degree as the child who does not get transferred and has four more weeks to come off O2. What effect does this have in cities that have multiple level II centres? Are they getting a fair comparison? If BPD is defined in such a way is it fair to include it in a composite outcome or if so perhaps it is best to stratify the comparisons to those centres with transfers to level II and those without.
Also with respect to BPD it is important to also note that the definition of BPD at 36 weeks is a matter of convenience. Drawing a line in the sand and declaring that this is when a child is labelled as having BPD allows us to compare ourselves with other units. It is a way of benchmarking. You will often hear Neonatologists say that we need to get a baby off O2 in the next few days as they approach 36 weeks as they want to have one less infant categorized as BPD. Let us not fool ourselves though. the infant who comes off O2 at 35 6/7 weeks gestational age has BPD in the sense that their lungs are not normal. The following day when they are off O2 the lungs have simply achieved a point at which the pulmonary reserve and alveolorization are sufficient to cope with room air breathing. The pulmonary tissue has not though improved greatly from one day to the next. What we need to focus on is minimizing the antecedent factors that lead to BPD rather than focusing our energy and quality work on getting these kids off O2 in the final days before 36 weeks. In so doing we make ourselves feel better but are the kids really any different?
Furthermore with respect to CLD as an outcome, it is not the same as it once was. My senior colleagues will well remember patients with tracheostomies dependent on a venitlator with sever BPD. The new BPD is a different animal. It is not something to be ignored but it is not the limiting factor any longer for most children in determining when they go home. It has been replaced by inability to take an infant’s oral intake by mouth for the most part. Establishing full feeds prior to discharge often takes a week or more after these same children have come off O2. To reduce length of stay efforts must be put into accelerating the time to full feeds. An example of this is semi-demand feeding which was the subject of another recent post.
In any event, I applaud the CNN for publishing another thought-provoking paper and it will be interesting to see what future research this may spark.
