What follows is a local news story that I had the pleasure of being involved in. I am posting on the blog not to show off in the least but rather highlight how true collaboration between professionals (who on the surface might not seem to be related) can accomplish incredible things. The strategy employed in this case had not been described before in the literature and thus it is my hope that this post may be shared at your local institutions and in the event a child with a cleft lip and palate is born and needs CPAP this appliance could be utilized.
If you would like further information on this approach please email me at [email protected] and I would be happy to provide you with assistance. The link to obtain the abstract and from there if you have personal or facility access to the full article can be found here: http://www.ncbi.nlm.nih.gov/pubmed/25794910
Within the last year a team of professionals from Dentistry, Neonatology and Respiratory Therapy came together to solve an unusual problem. A baby had been born prematurely at 26 weeks gestational age and less than 2 lbs and relied on a ventilator to help her breathe. As many of these children age, their reliance on a ventilator becomes less and they are changed to a non-invasive level of support called CPAP (continuous positive airway pressure). This consists of a mask put over the nose, which passes air into the lung thereby keeping a babies lungs inflated while we wait for continued development of their lungs. In this case however this premature infant had been born with a complete unilateral cleft lip and palate. Having this cleft created a leak, which makes the use of CPAP very challenging. The flow of air leaks out through the cleft instead of getting to the lungs to keep them inflated. One day, one of our respiratory therapists John Minski asked the Neonatologist on service (Dr. Michael Narvey) whether we could use a 3D scanning and printing technology to create an appliance that would seal the palate and allow pressure to be maintained in the lungs through the flow of air in the nose. Dr. Narvey had not heard of such a strategy being employed before but consulted Dr. Igor Pesun from the Faculty of Dentistry for an opinion and what came out of this discussion was a novel concept that we believe is the first of its kind.
A dental obturator was created to seal the palatal defect. 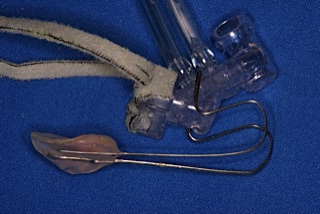 A child who is as small as Michaela, made the use of current intra oral scanning technology not possible. An impression using conventional dental materials was used to record the anatomy of the palate. A model was made and used to fabricate the obturator that was connected to the CPAP tubing.
A child who is as small as Michaela, made the use of current intra oral scanning technology not possible. An impression using conventional dental materials was used to record the anatomy of the palate. A model was made and used to fabricate the obturator that was connected to the CPAP tubing.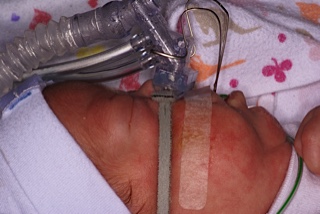
Over a period of 4 days the obturator was used to maintain a palatal seal and allowed for sufficient pressure to be maintained to manage the child off the ventilator. After this point she was deemed ready to transition to being off CPAP.
The collaboration between these services was instrumental in taking an idea from concept to reality. We were able to demonstrate that a premature infant, who previously would have been forced to remain on a ventilator until they were ready to come off breathing support completely, could be managed with a novel airway appliance. This type of approach has never been tried before in the literature and exemplifies some of the creative and innovative collaborative work happening at the Health Sciences Centre. Finally it serves as a shining example of how different seemingly unrelated specialties can come together within the Faculty of Health Sciences at the University of Manitoba.
