To many of you the answer is a resounding yes in that it reduces stress. Why is that though? Is it because you have had a personal experience that has been favourable, it is the practice in your unit or it just seems to make sense? It might come as a surprise to you who have followed this blog for some time that I would even ask the question but a social media friend of mine Stefan Johansson who runs 99NICU sent an article my way on this topic. Having participated in the FiCare study I realised that I have a bias in this area but was intrigued by the title of the paper. The study is Parental presence on neonatal intensive care unit clinical bedside rounds: randomised trial and focus group discussion by Abdel-Latif ME et al from New Zealand and was performed due to the lack of any RCTs on the subject specifically in the NICU.
Before I go on though I have to disclose a few biases.
- I love parents being on rounds so I can speak with them directly and have them ask me any questions they may have after hearing about their infants condition.
- Our unit encourages the practice.
- We are rolling out the principles of FiCare after being part of the study which encourages parental presence at the bedside for far more than just rounds.For information on implementing FiCare click here
- While this study is the only reported RCT on the subject in the NICU, the FiCare results will be published before long.
What is the problem with having families on rounds?
The detractors would say that sensitive information may be more difficult to discuss out in the open for fear that the family will take offence or be hurt. Another concern may be that teaching will be affected as the attending may not want to discuss certain aspects of care in order to prevent creating fear in the parents or awkwardness in the event that the management overnight was not what they would have done. Lastly, when patient volumes and acuity are high, having parents ask questions on rounds may lead to excessive duration of this process and lead to fatigue and frustration by all members of the team.
So what does this study add?
This particular study enrolled 72 families of which 63 completed the study. The study required 60 families to have enough power to detect the difference in having parents on rounds or not.The design was interesting in that the randomisation was a cross over design in which the following applied. One arm was having parents on rounds and the other without. The unit standard at the time was to not have parents on rounds.
≤30 weeks 1 week in one arm, one week washout period then one week in the other arm
>30 weeks 3 days in one arm, three day washout and then three days in the other arm
The primary outcome was to see if there would be a significant difference in the Parental Stressor Scale. 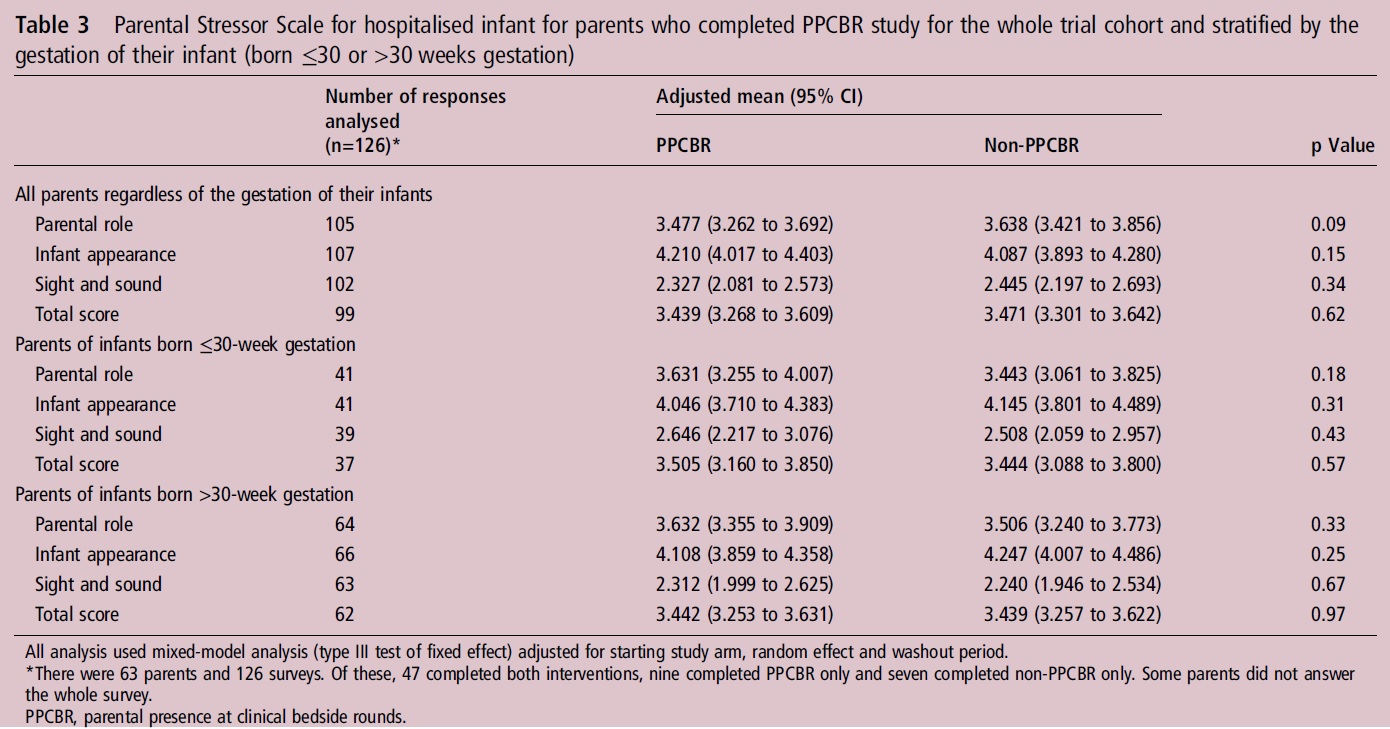
Surprisingly there was no difference across any domains of measuring parental stress. When we look at questions though pertaining to communication in the NICU we see some striking differences.
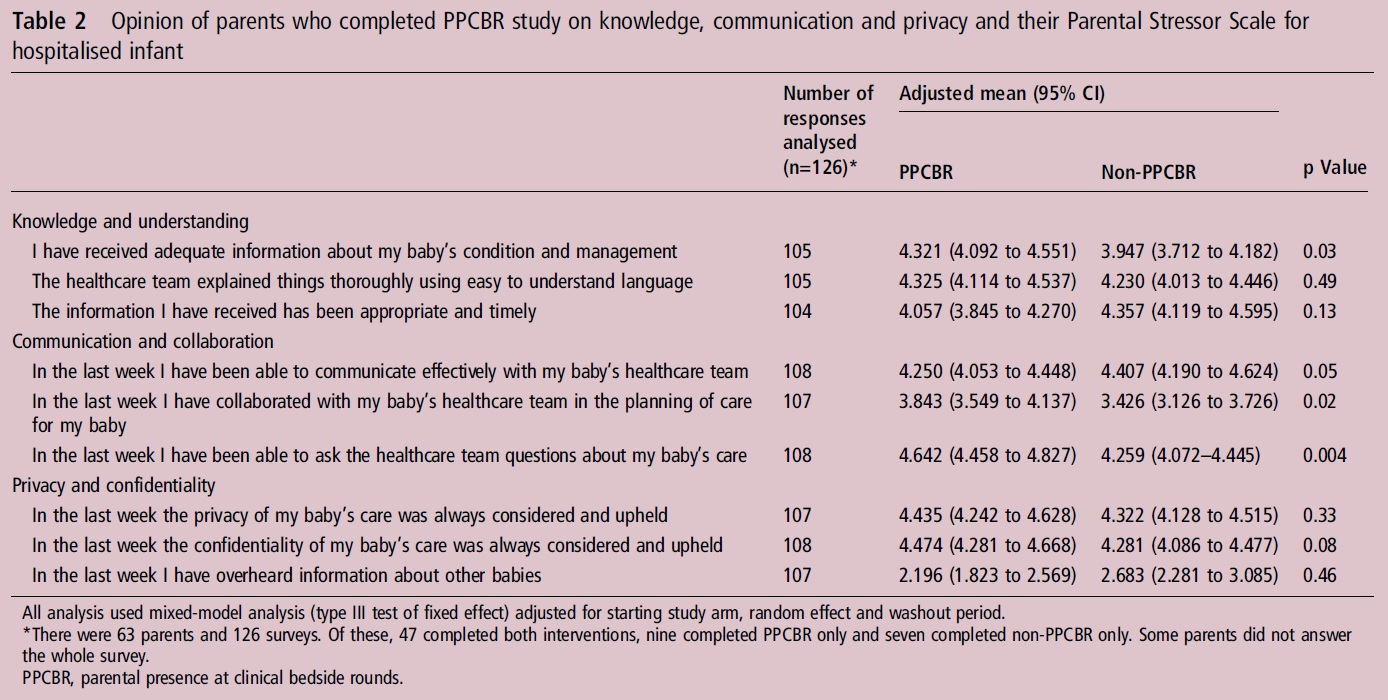
The families see many benefits to the model of being on rounds. They appear to have received more information, more contact with the team, contributed more to the planning of the course of their babies care and been able to ask more questions. All of these things would seem to achieve the goals of having parents on rounds.
So why aren’t parents less stressed?
This to me is the most interesting part of this post. The short answer is I am not sure but I have a few ideas.
- The study could not be blinded. If the standard of care in the unit was to not have parents on rounds, what kind of conversations happened after rounds? Were staff supportive of the families or were they using language that had a glass is half empty feel to it? Much like I am biased towards having parents on rounds and thanking them for their participation were there any negative comments that may have been unintentional thrown the families way.
- Is a little knowledge a dangerous thing? Perhaps as families learn more details about the care of their baby it gives them more things to worry about. Could the increase in knowledge while in some ways being pleasing to the family be offset by the concern that new questions raise.
- Was the intervention simply too short to detect a difference? This may have been a very important contributor. This short period of either a week or two leaves the study open to a significant risk that an event in either week could acutely increase stress levels. What if the infant had to go back on a ventilator after failing CPAP, needed to be reloaded with caffeine or developed NEC? With such short intervals one cannot say that while communication was better the parents were not stressed due to something unrelated to communication. In an RCT these should balance out but in such a small study I see this as a significant risk.
So where do we go from here?
I applaud the authors for trying to objectively determine the effect of parental presence on rounds in the NICU. Although I think they did an admirable job I believe the longer time frame of the FiCare study and the cluster randomised strategy using many Canadian centres will prove to be the better model to determine effectiveness. What the study does highlight though in a very positive way is that communication is enhanced by having parents on rounds and to me that is a goal that is well worth the extra time that it may take to get through rounds. Looking at it another way, we as the Neonatologists may need to spend less time discussing matters after rounds as we have taken care of it already. In the end it may be the most efficient model around!

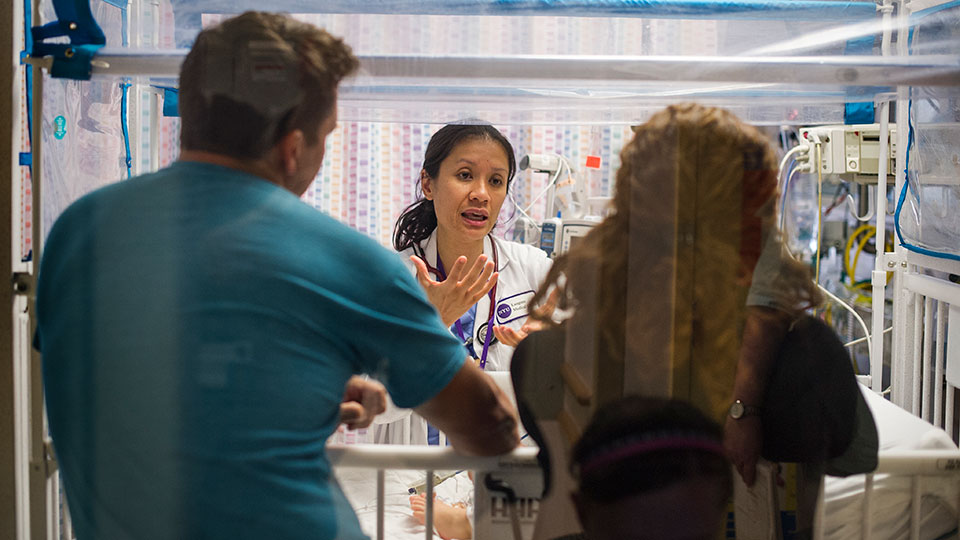
I will be very interested in seeing results from a much longer term study. While these are thought provoking I don’t think that looking at a few days to 2 weeks is enough time to say with any certainty that the results are valid over the long term. For instance, parents tend to experience increased stress when care providers change (neonatologist, residents, nurse practitioners) and that is frequently when erroneous communication about patients issues comes to light in rounds. A huge stressor for parents! This is also when care management strategies change due to neonatologist preferences which is also upsetting to parents.
The longer a family is in the NICU the more often they encounter these types of scenarios plus other issues that have the tendency to raise stress levels and sometimes cause trust issues.
Personally, I have always been torn at having parents present. Our unit allowed all parents to remain during rounds and I always felt this was an invasion of privacy. Mainly, at admission when maternal history was being discussed and sensitive information was verbalized within earshot of other parents. I continue to feel this a HIPPA violation.
I also did not enjoy seeing residents humiliated in front of parents under the guise of “teaching.” I don’t feel that is conducive to learning or to instilling trust in families.
In addition, I felt neonatologists used the time to their advantage so they did not have to talk to the families after rounds but this made for lengthy rounds and those who had to get orders written, exams done, tests ordered,etc were always running late and scrambling to get the work done. It was very common for rounds to last for hours and hours and run into the afternoon due to this propensity of neonatologists to showboat and chat with families.
Yes, it was great for families and if they missed rounds they were very disappointed but it was awfully hard on the worker bees.
I’m retired now and can only hope things have improved for my colleagues.
Wendy
Thank you for the comments. Agree with you longer term info is needed