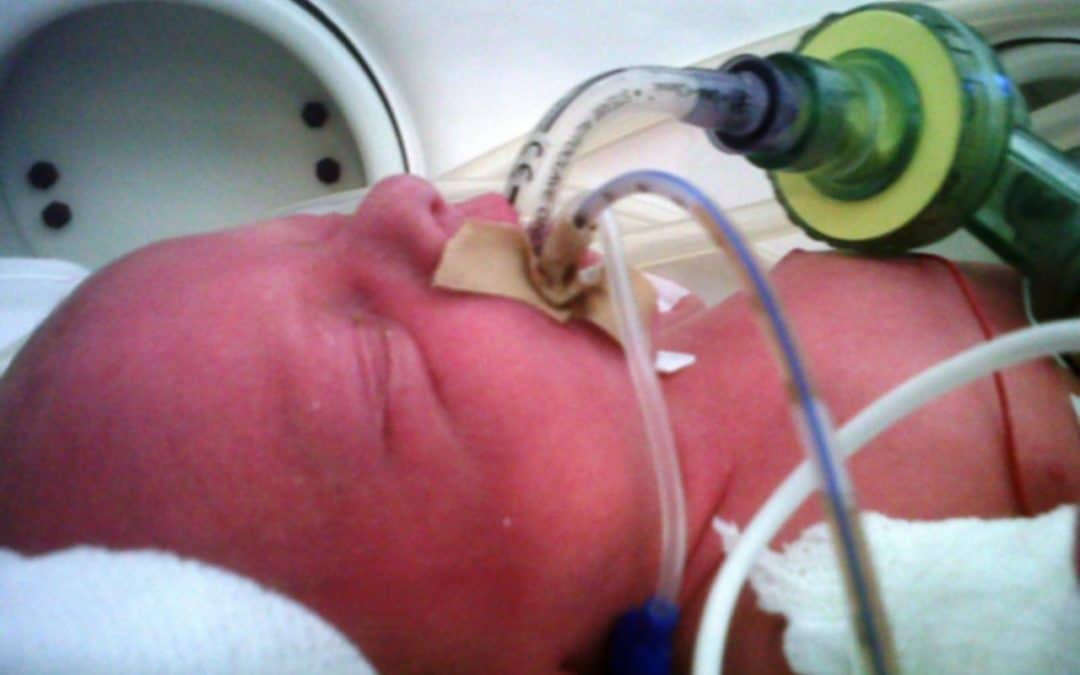
If I look back on my career there have been many things I have been passionate about but the one that sticks out as the most longstanding is premedicating newborns prior to non-emergent intubation. The bolded words in the last sentence are meant to reinforce that in the setting of a newborn who is deteriorating rapidly it would be inappropriate to wait for medications to be drawn up if the infant is already experiencing severe oxygen desaturation and/or bradycardia. The CPS Fetus and Newborn committee of which I am a member has a statement on the use of premedication which seems as relevant today as when it was first developed. In this statement the suggested cocktail of atropine, fentanyl and succinylcholine is recommended and having used it in our centre I can confirm that it is effective. In spite of this recommendation by our national organization there remain those who are skeptical of the need for this altogether and then there are others who continue to search for a better cocktail. Since I am at the annual conference for the CPS in Quebec city  I thought it would be appropriate to provide a few comments on this topic.
I thought it would be appropriate to provide a few comments on this topic.
Three concerns with rapid sequence induction (RSI) for premedication before intubation
1. “I don’t need it. I don’t have any trouble intubating a newborn” – This is perhaps the most common reason I hear naysayers raise. There is no question that an 60-90 kg practitioner can overpower a < 5kg infant and in particular an ELBW infant weighing < 1 kg. This misses the point though. Premedicating has been shown to increase success on the first attempt and shorten times to intubation. Dempsey 2006, Roberts 2006, Carbajal 2007, Lemyre 2009
2. “I usually get in on the first attempt and am very slick so risk of injury is less.” Not really true overall. No doubt there are those individuals who are highly successful but overall the risk of adverse events is reduced with premedication. (Marshall 1984, Lemyre 2009). I would also proudly add another Canadian study from Edmonton by Dr. Byrne and Dr. Barrington who performed 249 consecutive intubations with predication and noted minimal side effects but high success rates at first pass.
3. “Intubation is not a painful procedure”. This one is somewhat tough to obtain a true answer for as the neonate of course cannot speak to this. There is evidence available again from Canadian colleagues in 1984 and 1989 that would suggest that infants at the very least experience discomfort or show physiologic signs of stress when intubated using an “awake” approach. In 1984 Kelly and Finer in Edmonton published Nasotracheal intubation in the neonate: physiologic responses and effects of atropine and pancuronium. This randomized study of atropine with or without pancuronium vs control demonstrated intracranial hypertension only in those infants in the control arm with premedication ameliorating this finding. Similarly, in 1989 Barrington, Finer and the late Phil Etches also in Edmonton published Succinylcholine and atropine for premedication of the newborn infant before nasotracheal intubation: a randomized, controlled trial. This small study of 20 infants demonstrated the same finding of elimination of intracranial hypertension with premedication. At the very least I would suggest that having a laryngoscope blade put in your oral cavity while awake must be uncomfortable. If you still doubt that statement ask yourself whether you would want sedation if you needed to be intubated? Still feel the same way about babies not needing any?
4. What if I sedate and paralyze and there is a critical airway? Well this one may be something to consider. If one knows there is a large mass such as a cystic hygroma it may be best to leave the sedation or at least the paralysis out. The concern though that there might be an internal mass or obstruction that we just don’t know about seems a little unfounded as a justification for avoiding medications though.
Do we have the right cocktail?
The short answer is “I don’t know”. What I do know is that the use of atropine, an opioid and a muscle relaxant seems to provide good conditions for intubating newborns. We are in the era of refinement though and as a recent paper suggests, there could be alternatives to consider;Effect of Atropine With Propofol vs Atropine With Atracurium and Sufentanil on Oxygen Desaturation in Neonates Requiring Nonemergency IntubationA Randomized Clinical Trial. I personally like the idea of a two drug combination for intubating vs.. three as it leaves one less drug to worry about a medication error with. There are many papers out there looking at different drug combinations. This one though didn’t find a difference between the two combinations in terms of prolonged desaturations between the two groups which was the primary outcome. Interestingly though the process of intubating was longer with atropine and propofol. Given some peoples reluctance to use RSI at all, any drug combination which adds time to the the procedure is unlikely to go over well. Stay tuned though as I am sure there will be many other combinations over the next few years to try out!

In NSW Australia we commonly use Morphine 5mins Atropine and Sux
I personally leave out the atropine in the tachycardic septic baby.
This regime works well.
I have had difficulty with fentanyl and chest wall rigidity – admittedly this maybe because of the rapid onset of action – do you chase it with sux? I know there is a lot of literature saying that fentanyl is superior to morphine but when I try to change practice my baby goes blue, teaching goes out the window and I have to intubate quick smart!
We have had a death in NSW using propofol in the newborn – unlikely to get up again in my generation. It was used in a baby already on prostin and preterm so profound hypotension may have been predictable but we are now gun shy. Thanks for the thought provoking topic.
What is your cocktail of choice? We use fentanyl, atropine and rocuronium. I have had only once instance of chest wall rigidity with this and it was an anxious nurse who pushed the fentanyl instead of administering it in the usual manner but administering the rocuronium cleared that up. Another argument I had heard is that it prevents in and out surfactant admin. Given that I always tape and tube and obtain an x Ray before giving surfactant that’s not an issue for me and many are typically awake enough within 1-2 hours to wean rapidly and extubate.
we use atropine, fentanyl and succinylcholine. Works well without a prolonged paralysis
What dose of Fentanyl do tou use for “INSURE” ?
3 mcg/kg
4 drugs:
Atropin
Wait 10-15 min
Fentanyl real slow, at least 5 min, followed by slow sodium flush
Take over the babies breathing by mask ventilation
Thiopental
Flush
Suxameton
Flush
Intubate!
You will never fail…
Baby is a sleep and pain is prevented.
Insightful article,
We use Fentanyl and Midazolam, for sedation and analgesia beforehand elective intubation.
But for surfactant delivery, sedation before procefure was associated with lot of apneas.
In Nepean Hospital NSW Australia we use three drugs for premedication.
Morphine 100 mcg/kg
Atropine 10 mcg/kg and
Suxamethonium 1-2 mg/kg.
With premeditation intubation happens quickly and successfully with minimal pain to baby.
In case of In and out Surfactant we use lesser dose of morphine at 50 mcg/kg + Atripine and Suxamethonium as above.
I always use premeditation for non emergent intubation and it’s good for baby as well.
Our greatest challenge is not related to skill, success, or ignorance to pain, but rather the desire to administer “in & out” surfactant and extubate immediately back to CPAP. This population comprises most of our non-emergent intubations, and is also the population we don’t want to leave on a vent just because they are sedated.
for those babies I have used atropine and fentanyl with succ on standby. If needed one can reverse with naloxone but thus far I haven’t needed it
according NRP 2016 NO NEED TO SEDATION, but if you want to wait untill drug effect started its too late ,i dont need to sedat
I agree that in the acute situation as in an NRP resuscitation there is no need for such medications although some work is starting looking at intranasal use of medications. In the semi-elective intubation that is where I argue we should definitely use meds
The topic is about non-emergency intubation while NRP is all about emergency intubation during resuscitation of a newborn
I hear you and share your concern if a practitioner is overly confident. If its been proven that the medication is safe, then I agree why struggle with in infant that is merely naturally reacting to somthing that feels uncomforatable and unnatural to him or her. It is not merely about the pactioners confindence aside from that we are speaking of babies. Delicate sensative little wonderful and beatuful little human beings with the same ability to feel fear and discomfort. Their comfort level is so important. Somthing to consider.
very well said Amy
From my practice l usually use dormicum as stat dose 0.3mg/kg
Then intubate the baby after that put baby on morphine infusion with attraction or fentanyl or Formica infusion with close monitor to the baby.
we don’t have access to dormicum
But what of Surfactant via a fine catheter approach? Meta-analyses of six trials show reduction in BPD/ Death as well as other morbidities.. and sedation not mandated and was typically not used in these trials….
Would a bit of discomfort be considered OK if it resulted in improved outcomes by motioning spontaneous breathing?
Indeed David I agree with you about LISA techniques. This has been slow to adopt despite the evidence pointing to better outcomes. I suspect it is a little bit of there being resistance to “teaching old dogs new tricks” but yes it would be difficult to premedicate. Perhaps lower doses to “take the edge off” such as giving atropine followed by 2 mcg/kg of fentanyl might be considered but apnea would of course make this difficult to do if even at lower fentanyl doses drive was lost
As a neonatal fellow, I presented this topic as an exhaustive journal review to faculty. I’d like to begin by saying that we have an amazing group with experience spanning from 6 yrs to 40 years – and they all were unanimous in the idea that although there is data out there – there is not much utility to paralysing the <1500 grams. Yes to the term PPHN babies but not so much otherwise.
In personal experience, I feel pro- RSI in non-emergent situations, even for the little ones.
I may have a long road to tread before deciding what I would pursue in practice, but it certainly made for an interesting talk. Also – I would like to say 'Thank you' because I gained the idea for my journal review from your blog :).
That is a really inspriational thing to say. Happy to help contribute to your learning